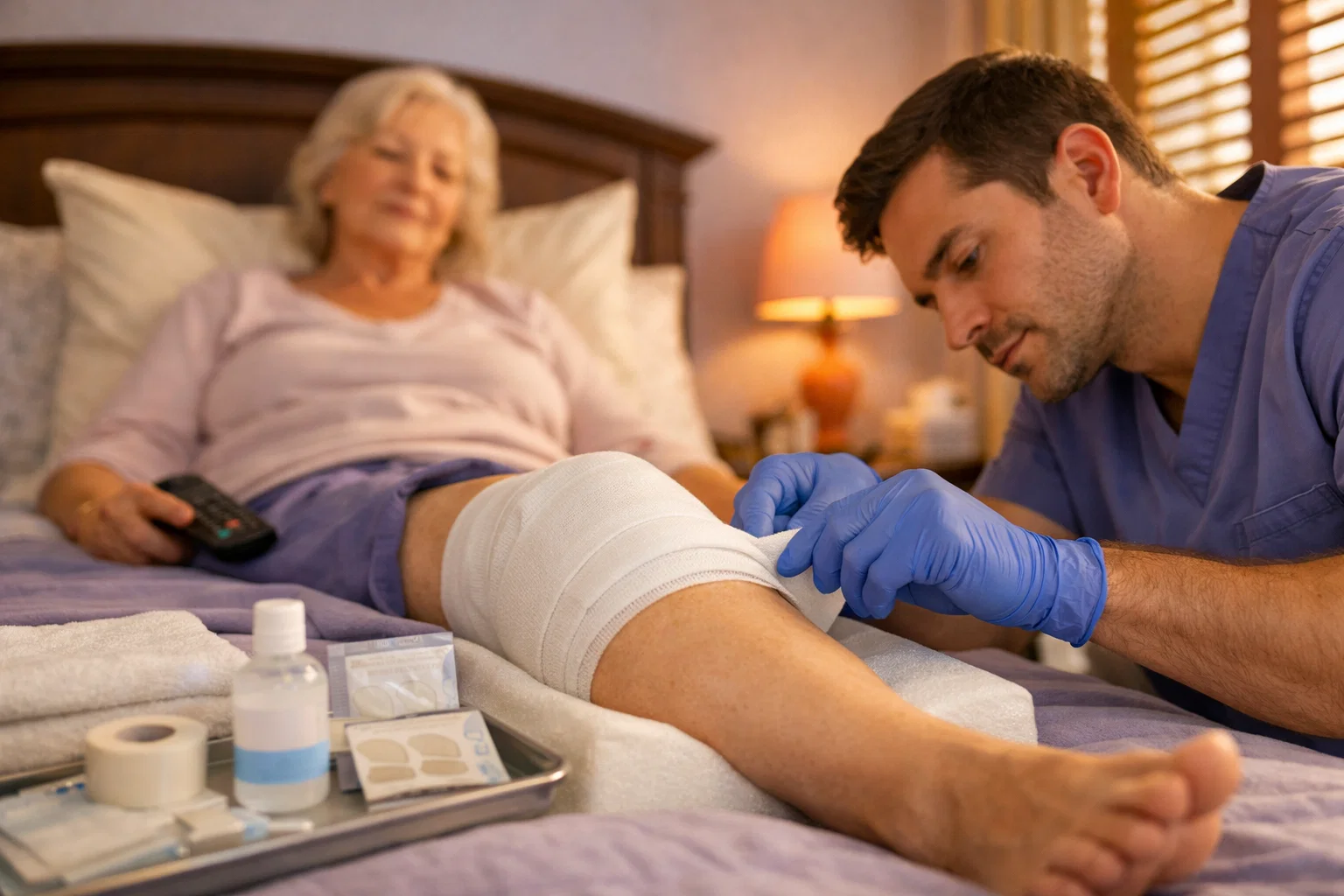
Hip and knee replacement surgeries are among the most common procedures performed in the United States. Recovery at home is possible for most patients — but the surgical wound left behind requires expert monitoring and care. Infections, wound separation, and prolonged drainage are among the most serious complications after joint replacement. Fortunately, Medicare covers skilled nursing wound care at home at $0 cost for qualifying patients.
HarvardCare at Home provides specialized post-surgical wound care throughout Los Angeles County. Visit our Medicare wound care in Los Angeles page and our post-surgical wound care at home service to learn more.
Why Joint Replacement Wounds Need Professional Care
Hip and knee replacements involve large incisions — typically 6 to 10 inches. As a result, healing is complex and the risk of complications is real. Surgical site infections after joint replacement affect approximately 1–2% of patients. However, when they occur, they are devastating. Treatment often requires additional surgery, prolonged antibiotic courses, or in severe cases, implant removal.
Professional wound monitoring catches problems early — when they are still manageable. Additionally, proper wound care technique reduces infection risk significantly compared to self-care by untrained caregivers. In-home nursing eliminates the need to travel to a clinic while your wound is fresh and mobility is limited. That is a significant advantage in Los Angeles, where outpatient clinic visits can take hours.
Common Complications Our Nurses Watch For
Surgical Site Infection
Infection is the most feared complication after joint replacement. It can be superficial — affecting skin and subcutaneous tissue — or deep, involving the joint itself. Deep infections may require implant removal. Early signs include increasing redness, warmth, swelling, pain beyond what’s expected, and drainage with odor. Specifically, our nurses assess for all infection signs at every wound care visit and contact your surgeon immediately when warning signs appear. For more, read our guide on signs your wound is infected and what to do next.
Wound Dehiscence
Wound dehiscence — the partial or complete opening of a surgical incision — occurs when wound edges separate before adequate healing. It is more common in patients with diabetes, obesity, or malnutrition. Additionally, patients who take corticosteroids face higher risk. A dehisced wound requires prompt professional assessment and treatment. In some cases, wound VAC therapy is indicated to support closure. Our wound VAC therapy at home team manages dehiscence using evidence-based protocols.
Seroma and Hematoma
Seromas (fluid collections) and hematomas (blood collections) are common after joint replacement. Small collections often resolve on their own. However, large or expanding collections may require intervention and increase infection risk. Our nurses monitor drainage, measure any swelling around the incision, and communicate with your orthopedic surgeon when intervention may be needed.
Persistent Wound Drainage
Some drainage in the first few days after surgery is normal. However, persistent drainage beyond 5–7 days is a warning sign. It increases infection risk and may indicate a deeper problem. Specifically, persistent drainage after total knee replacement is associated with higher rates of deep infection. Therefore, our nurses track drainage characteristics at every visit and escalate to the surgeon when indicated.
What Wound Care Services Does Medicare Cover After Joint Replacement?
Medicare covers skilled nursing wound care at home after hip or knee replacement for homebound patients. Covered services include wound assessment and measurement at every visit, dressing changes using clinically appropriate materials, wound cleansing and irrigation, monitoring for infection and other complications, staple or suture removal when ordered, drain management for surgical drains, and caregiver education on wound monitoring between visits.
Additionally, under Medicare Part B’s surgical dressing benefit, wound dressings for post-surgical wounds are also covered. Our wound dressing changes at home and wound care nurse at home services cover all of these interventions. For the full picture of Medicare wound care coverage, visit our Medicare wound care in Los Angeles page.
Do You Qualify for Home Wound Care After Joint Replacement?
Most patients discharged home after hip or knee replacement qualify for Medicare home health wound care. You must be enrolled in Medicare, be homebound, need skilled nursing wound care ordered by your surgeon or physician, and receive care through a Medicare-certified agency. Homebound status is almost always satisfied immediately after joint replacement. Getting in and out of a car is painful. Walking requires a device. Leaving home is a taxing effort — which meets Medicare’s definition exactly.
For full eligibility details, read our guides on what qualifies as homebound for Medicare and how to get home health care through Medicare.
Wound Care and Physical Therapy: A Coordinated Approach
After joint replacement, wound care nursing and physical therapy work hand in hand. Your wound care nurse monitors the surgical site and manages the incision. Meanwhile, your physical therapist rebuilds strength, mobility, and function. Both services are covered by Medicare at $0 cost. Furthermore, this coordinated approach produces better outcomes than either service alone — the therapist monitors functional progress while the nurse ensures the wound is not compromised by rehabilitation exercises.
HarvardCare at Home provides both services under a unified plan of care. Our hip replacement rehab at home and knee replacement rehab at home programs include wound care nursing when indicated. Read our recovery guides: recovery after hip replacement week by week and knee replacement recovery guide.
Dressing Types Used for Joint Replacement Wounds
The right dressing depends on the wound’s healing stage and drainage level. In the early postoperative period, absorbent non-adherent dressings manage drainage while protecting the wound. As drainage decreases, moisture-retentive dressings support the final stages of closure. For wounds with dehiscence or excessive drainage, foam dressings, alginate dressings, or wound VAC therapy may be indicated. Importantly, our nurses select dressings based on evidence-based wound assessment at every visit — never a one-size-fits-all approach. Read our guides on caring for surgical wounds at home and how to make your incision heal faster.
Wound Healing Timeline After Joint Replacement
Understanding what’s normal helps patients recognize concerning changes early. In the first 1–3 days, some drainage, swelling, and bruising is expected. By days 4–7, drainage should decrease significantly and wound edges should be coming together. In weeks 2–3, the wound should be closing and staples or sutures may be removed. By week 6, most surgical wounds are well healed at the surface — though deeper tissue healing continues for months. However, any increase in redness, drainage, pain, or warmth at any stage warrants immediate professional assessment. Read our guide on how long a wound takes to heal by type for a detailed timeline.
Nutrition and Joint Replacement Wound Healing
Nutrition plays a critical role in surgical wound healing. Protein is the most important nutrient — it is required to synthesize new collagen and support immune defense. Vitamin C is essential for collagen cross-linking. Zinc supports immune function and cell proliferation. Additionally, adequate hydration maintains tissue perfusion. As a result, our nurses routinely assess nutritional status and provide education at every visit. Read our guides on 10 foods that speed up wound healing and the impact of nutrition on wound healing in older adults for specific dietary guidance.
Diabetes and Joint Replacement Wound Complications
Patients with diabetes face significantly higher risks after joint replacement surgery. Elevated blood sugar impairs immune function and slows collagen synthesis. As a result, wounds heal more slowly and infection risk is higher. Specifically, HbA1c levels above 7.5–8% at the time of surgery are associated with substantially higher complication rates. Our wound care nurses monitor blood glucose trends, assess for signs of early infection vigilantly, and coordinate with both the orthopedic surgeon and endocrinologist or primary care physician when needed. Read our related guides on the connection between diabetes and slow wound healing and managing diabetes to prevent foot complications.
Getting Started With Post-Surgical Wound Care at Home
Before leaving the hospital after joint replacement, ask your surgeon to include home health wound care in your discharge orders. Specifically, request orders for a Medicare-certified home health agency to provide skilled nursing wound care and physical therapy. Your discharge planner can also help coordinate this transition. HarvardCare at Home accepts referrals directly from orthopedic surgeons, hospitals, and surgical centers throughout LA County. Our first visit occurs within 48 hours of referral receipt.
We serve post-surgical wound care patients across Los Angeles County — including Los Angeles, Beverly Hills, Santa Monica, Pasadena, Glendale, Torrance, and beyond. Visit our post-hospital discharge nursing page and our Medicare wound care in Los Angeles page. To get started, contact our team or review our frequently asked questions.
How to Prepare Your Home for Post-Surgical Wound Care
Before your first wound care visit, a few simple preparations make the process smoother. First, make sure your nurse has easy access to the wound area — lay out comfortable clothing that allows access without difficulty. Second, have a clean, well-lit space where dressing changes can be performed. Third, keep a list of your current medications and any wound care supplies you received at discharge. Additionally, write down any questions or concerns you have about your wound — our nurses welcome detailed questions and take time to answer them at every visit. Furthermore, if you have a caregiver at home, encourage them to be present during wound care visits. As a result, they learn proper wound monitoring between nursing visits. Read our guide on preparing your home for post-surgery recovery for a complete preparation checklist.
Preventing Infection: What You Can Do Between Visits
Your wound care nurse provides expert treatment at each visit. However, the hours between visits also matter. Several steps reduce infection risk between nursing visits. First, keep the wound covered with the dressing your nurse applied — do not remove it early unless it becomes saturated or falls off. Additionally, keep the wound dry unless your nurse instructs otherwise. Avoid soaking in a bath, pool, or hot tub until your nurse or surgeon clears you. Furthermore, wash your hands thoroughly before touching the wound area for any reason. Watch for warning signs between visits — increasing redness, warmth, swelling, or drainage that soaks through the dressing. Specifically, if you develop a fever above 101°F, contact your surgeon immediately. In general, trust your instincts — if something looks or feels wrong, call your nurse or surgeon right away. Read our full guide on surgical wound care: what to know after an operation.
Frequently Asked Questions
How many wound care visits will I need after joint replacement? Most uncomplicated wounds require 3–5 nursing visits over 2–3 weeks. Complex wounds with drainage, dehiscence, or infection may require daily or multiple-times-weekly visits for 4–8 weeks or longer.
Does Medicare cover wound care after knee replacement if I also had a vein harvested? Yes — Medicare covers wound care for all surgical sites from a single procedure. Both the knee incision and any vein harvest site wounds are covered under the home health benefit.
Can I receive wound care and physical therapy on the same day? Yes. In fact, coordinating same-day visits is often the most efficient approach. HarvardCare at Home coordinates scheduling to minimize separate visit days when clinically appropriate.
What if my wound isn’t healing after 4 weeks? A wound that hasn’t shown measurable progress after 4 weeks is considered at risk of becoming chronic. Specifically, consult with your surgeon and ask about a referral to a wound care specialist. Your home health nurse will document wound measurements at every visit so progress — or lack of it — is clearly tracked over time. Read our guide on why won’t my wound heal for common reasons healing stalls.
 HarvardCare at Home
HarvardCare at Home