A wound is considered chronic when it fails to progress through normal healing stages within four to six weeks despite appropriate treatment. Chronic wounds often become stuck in the inflammatory phase, unable to build new tissue and close. Underlying factors like poor circulation, diabetes, pressure, infection, or nutritional deficiencies typically prevent healing. Identifying and addressing these barriers is essential for chronic wound resolution.
WOUND CARE
Chronic Wound Care at Home
Chronic wound care at home throughout Los Angeles County. Our specialists treat non-healing wounds including venous ulcers, arterial ulcers, pressure injuries, and surgical wound complications using advanced therapies. Medicare accepted.
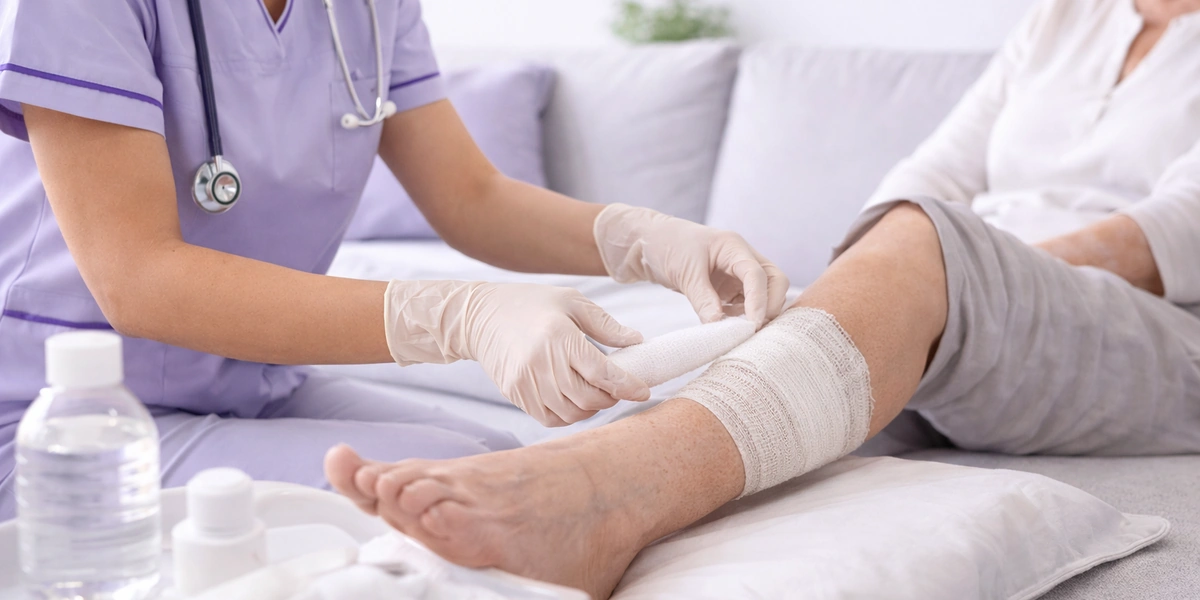
Specialized Treatment for Wounds That Will Not Heal
When a wound persists for weeks or months despite treatment, frustration and fear set in. You have tried everything your doctor suggested, followed all the instructions, yet the wound remains open, draining, and refusing to heal. Chronic wounds—those that fail to progress through normal healing stages within four to six weeks—require specialized intervention beyond standard wound care. At HarvardCare at Home, our chronic wound specialists bring advanced treatment directly to patients throughout Los Angeles County, offering hope and healing for wounds that have resisted conventional approaches.
Chronic wounds affect approximately 6.5 million Americans and represent one of the most challenging problems in healthcare. These wounds drain healthcare resources, diminish quality of life, cause persistent pain, and carry serious risks including infection, hospitalization, and amputation. Yet with expert intervention addressing the underlying causes of non-healing, most chronic wounds can eventually close. Our home-based chronic wound care program delivers that expert intervention where patients are most comfortable—in their own homes.
Understanding Chronic Wounds
Normal wound healing follows a predictable sequence of phases: inflammation clears debris and fights infection, proliferation builds new tissue, and remodeling strengthens the repair. Chronic wounds become stuck in one of these phases, typically inflammation, unable to progress toward closure.
Why Wounds Become Chronic
Multiple factors can interrupt normal healing and create chronic wounds. Underlying medical conditions like diabetes, vascular disease, and autoimmune disorders impair the body’s healing capacity. Poor circulation deprives wounds of oxygen and nutrients essential for tissue repair. Persistent infection keeps wounds in the inflammatory phase indefinitely. Repeated trauma from pressure or friction continuously damages fragile new tissue. Nutritional deficiencies leave the body without building blocks for repair. Certain medications suppress immune function or impair healing processes. Often, multiple factors combine to create wounds that simply cannot heal without addressing each barrier.
The Chronic Wound Cycle
Chronic wounds often fall into a self-perpetuating cycle. The wound produces excessive inflammatory chemicals that break down new tissue as fast as it forms. Bacterial colonization, even without overt infection, triggers ongoing inflammation. The wound bed becomes filled with non-viable tissue that prevents healthy tissue growth. Without intervention to break this cycle, the wound persists indefinitely—or worsens.
Types of Chronic Wounds We Treat
Our chronic wound care program addresses all major categories of non-healing wounds.
Venous Leg Ulcers
When veins in the legs cannot efficiently return blood to the heart, pressure builds in the lower leg tissues, eventually causing skin breakdown and ulceration. Venous ulcers typically appear on the inner lower leg, often around the ankle. They tend to be shallow with irregular borders and produce significant drainage. Treatment requires addressing the underlying venous insufficiency through compression therapy while simultaneously managing the wound itself.
Arterial Ulcers
Arterial ulcers result from inadequate blood flow to the tissues, usually due to peripheral arterial disease. They commonly appear on the feet, toes, or lower legs and tend to be deeper with well-defined edges. The surrounding skin often appears pale or mottled, and the limb may be cool to touch. Arterial wounds require careful management because compression—helpful for venous wounds—can be harmful when arterial flow is compromised. Treatment often requires vascular intervention to restore blood flow before the wound can heal.
Pressure Ulcers
Pressure ulcers develop when sustained pressure cuts off blood supply to tissues, causing cell death and skin breakdown. They occur over bony prominences—the sacrum, heels, hips, and other areas where bone meets surface during sitting or lying. Pressure ulcers range from superficial skin damage to deep wounds extending to muscle and bone. Treatment requires both wound management and pressure elimination through repositioning, support surfaces, and offloading devices.
Non-Healing Surgical Wounds
Sometimes surgical incisions fail to heal as expected, breaking down days or weeks after the procedure. Factors contributing to surgical wound dehiscence include infection, poor nutrition, diabetes, obesity, and excessive tension on the wound. These wounds require careful management to promote healing by secondary intention while monitoring for complications.
Radiation Wounds
Radiation therapy can damage skin and underlying tissues, sometimes causing wounds that appear months or years after treatment ends. Radiation wounds are particularly challenging because the affected tissues have compromised blood supply and reduced healing capacity. Specialized techniques are often required to promote healing in irradiated tissue.
Inflammatory and Autoimmune Wounds
Conditions like pyoderma gangrenosum, vasculitis, and other inflammatory disorders can cause wounds that resist standard treatment. These wounds require management of the underlying inflammatory condition alongside local wound care.
Our Chronic Wound Care Approach
Healing chronic wounds requires a systematic approach that addresses all barriers to healing simultaneously.
Comprehensive Wound Assessment
Effective chronic wound treatment begins with thorough assessment. We evaluate the wound itself—size, depth, tissue types present, drainage characteristics, and signs of infection. We assess the wound edges and surrounding skin. We examine circulation through pulse assessment and other indicators. We review your complete medical history, medications, nutritional status, and previous treatments. This comprehensive picture reveals why your wound has not healed and guides our intervention strategy.
Identifying and Addressing Barriers
Based on assessment findings, we develop a plan to address every factor impeding healing. This may include optimizing blood sugar control for diabetic patients, implementing compression therapy for venous insufficiency, coordinating vascular evaluation for arterial disease, addressing nutritional deficiencies through dietary guidance, reviewing medications that may impair healing, and ensuring adequate pressure redistribution for pressure wounds. Addressing these systemic factors is as important as the wound treatment itself.
Wound Bed Preparation
Chronic wounds typically contain devitalized tissue, excessive bacteria, and abnormal wound fluid that prevent healing. Wound bed preparation clears these obstacles through debridement to remove dead and dying tissue, biofilm disruption to address bacterial colonies, moisture management to maintain optimal wound environment, and edge treatment to stimulate stalled wound margins. This preparation converts a chronic wound into one capable of progressing through normal healing phases.
Advanced Wound Therapies
When standard approaches prove insufficient, we employ advanced wound care modalities:
- Negative pressure wound therapy draws fluid from wounds, reduces bacterial burden, and stimulates tissue growth
- Bioengineered skin substitutes provide scaffolding and growth factors for tissue regeneration
- Growth factor applications stimulate cellular activity in stalled wounds
- Advanced antimicrobial dressings address bacterial colonization without systemic antibiotics
- Collagen and matrix products support tissue regeneration
- Hyperbaric oxygen referral when appropriate for wounds requiring enhanced oxygen delivery
Appropriate Dressing Selection
No single dressing works for all wounds or all stages of healing. We select dressings based on wound characteristics—moisture level, depth, infection status, drainage amount, and location. As your wound evolves, dressing selection evolves with it. Our expertise in dressing selection ensures your wound maintains optimal healing conditions at every stage.
Infection Management
Chronic wounds are highly susceptible to infection, and infection is a leading cause of wound chronicity. We monitor vigilantly for signs of infection, obtain cultures when indicated, and coordinate with physicians for appropriate antibiotic therapy. We also address biofilm—communities of bacteria that resist standard treatment—through specialized debridement and antimicrobial approaches.
Pain Management
Chronic wounds often cause significant pain that affects quality of life and can impede healing. We address wound-related pain through appropriate dressing selection to minimize trauma during changes, timing of care relative to pain medication, gentle techniques that respect sensitive tissues, and coordination with physicians for adequate pain control. Reducing pain not only improves comfort but supports the healing process.
The Journey to Healing
Healing chronic wounds takes time and persistence. We set realistic expectations from the start and track progress meticulously.
Establishing Baseline and Goals
At your first visit, we document detailed wound measurements, photographs, and characteristics. We discuss realistic timelines and establish measurable goals. While complete healing is always the ultimate objective, intermediate goals—wound size reduction, improved tissue quality, decreased drainage—demonstrate progress and guide treatment adjustments.
Regular Reassessment
We reassess your wound at every visit, tracking changes in size, depth, and tissue characteristics. Wounds that are not progressing trigger treatment plan review and adjustment. We share progress reports with your physician regularly and communicate promptly about any concerns.
Treatment Adjustment
Chronic wound care is not static. As your wound responds—or fails to respond—we adjust our approach. Dressings change as wound characteristics evolve. Advanced therapies are introduced when needed. Systemic factors are revisited if healing stalls. This dynamic, responsive approach maximizes your chances of successful healing.
Benefits of Home-Based Chronic Wound Care
For chronic wounds requiring long-term management, home-based care offers particular advantages.
Consistency of Care
Chronic wounds require consistent, ongoing treatment. Home care removes transportation barriers that can lead to missed appointments and treatment gaps. Your nurse knows your wound intimately and tracks subtle changes over time.
Reduced Infection Risk
Patients with chronic wounds are vulnerable to infection. Receiving care at home minimizes exposure to pathogens found in healthcare facilities.
Comprehensive Home Assessment
For pressure wounds and wounds affected by mobility limitations, your home environment matters. Home-based care allows assessment and modification of factors in your living space that affect healing.
Improved Adherence
When we see your actual situation—how you move, where you sit, what you eat—we can make practical recommendations you can actually follow. This realistic approach improves adherence to the complete treatment plan.
Coverage and Getting Started
Chronic wound care services are covered by Medicare, Medi-Cal, and most insurance plans when ordered by a physician. Given the complexity and duration of chronic wound treatment, our team works closely with insurers to ensure continued authorization and coverage.
If you have a wound that has not healed despite weeks or months of treatment, do not lose hope. Contact HarvardCare at Home today for a free assessment. Our chronic wound specialists are ready to evaluate your wound, identify barriers to healing, and implement a comprehensive treatment plan—all in the comfort of your own home. Healing is possible, and we are here to help you achieve it.
FAQs
Do you have questions?
Got questions about Chronic Wound Care at Home? Here are answers to what patients and families ask most.
Chronic wounds persist because something is preventing normal healing—and that barrier has not been adequately addressed. Common causes include uncontrolled diabetes affecting tissue repair, vascular disease limiting blood flow, ongoing pressure or friction traumatizing the wound, hidden infection or biofilm, nutritional deficiencies, or medications that impair healing. Our comprehensive assessment identifies these barriers so treatment can address them directly.
Beyond standard dressings, chronic wounds may benefit from negative pressure wound therapy, bioengineered skin substitutes, growth factor applications, advanced antimicrobial dressings, collagen matrices, and specialized debridement techniques. Some patients require hyperbaric oxygen therapy. We determine which advanced modalities are appropriate based on your specific wound characteristics and response to treatment.
Healing time varies greatly depending on wound size, depth, location, underlying causes, and your overall health. Some chronic wounds heal in weeks once barriers are addressed. Others require months of treatment. Very complex wounds may take a year or longer. We set realistic expectations based on your specific situation and track progress closely, adjusting treatment when wounds are not improving as expected.
Unfortunately, yes—untreated or poorly managed chronic wounds, particularly on the feet and legs, can lead to infections that spread to bone or become life-threatening, sometimes requiring amputation to save a life. This is why chronic wound care is so important. With appropriate treatment addressing all healing barriers, most chronic wounds can eventually heal and amputation can often be avoided.
TESTIMONIALS
What Our Patients & Families Say
AREAS WE SERVE
Chronic Wound Care at Home Near You
Our licensed healthcare professionals provide expert care in the comfort of your home. We proudly serve patients and families throughout Los Angeles County.
- A
- Agoura Hills
- Alhambra
- Altadena
- Arcadia
- B
- Bel Air
- Bellflower
- Beverly Hills
- Boyle Heights
- Brentwood
- Burbank
- C
- Calabasas
- Carson
- Century City
- Cerritos
- Claremont
- Compton
- Covina
- Culver City
- D
- Diamond Bar
- Downey
- E
- Eagle Rock
- East Los Angeles
- Echo Park
- Encino
- G
- Gardena
- Glendale
- Glendora
- Granada Hills
- H
- Hacienda Heights
- Hancock Park
- Harbor City
- Hawthorne
- Highland Park
- Hollywood
- Hollywood Hills
- I
- Inglewood
- K
- Koreatown
- L
- La Crescenta-Montrose
- La Mirada
- Lakewood
- Lincoln Heights
- Long Beach
- Los Angeles
- Los Feliz
- M
- Malibu
- Manhattan Beach
- Mar Vista
- Marina del Rey
- Mid-City
- Mid-Wilshire
- Miracle Mile
- Monrovia
- Montebello
- Monterey Park
- N
- North Hollywood
- Northridge
- Norwalk
- P
- Pacific Palisades
- Palms
- Palos Verdes Estates
- Palos Verdes Peninsula
- Panorama City
- Pasadena
- Pico Rivera
- Playa Vista
- Pomona
- Porter Ranch
- R
- Rancho Palos Verdes
- Redondo Beach
- Reseda
- Rolling Hills Estates
- Rowland Heights
- S
- San Dimas
- San Gabriel
- San Marino
- San Pedro
- Santa Clarita
- Santa Monica
- Sawtelle
- Sherman Oaks
- Silver Lake
- South Gate
- South Pasadena
- Studio City
- T
- Tarzana
- Torrance
- V
- Van Nuys
- Venice
- W
- West Covina
- West Hollywood
- West Los Angeles
- Westchester
- Westlake Village
- Westwood
- Whittier
- Wilmington
- Woodland Hills
More Services
In-Home Wound Care Services
- Board-certified wound care nurses
- Personalized treatment plans
- All wound types treated
Diabetic Wound Care at Home
- Diabetes wound specialists
- Blood sugar optimization support
- Advanced offloading techniques
Skilled Nursing Care at Home
- Registered nurses available 7 days a week
- Comprehensive care coordination
- IV therapy and infusion services