Dressing change frequency depends on wound type, drainage level, and the dressing products used. Some wounds need daily changes, while others do well with changes every two to three days. Certain modern dressings can stay in place up to seven days. Your nurse determines the appropriate frequency based on wound assessment and adjusts it as healing progresses. More drainage or infection concerns may require more frequent changes.
WOUND CARE
Wound Dressing Changes at Home
Professional wound dressing changes at home throughout Los Angeles County. Our skilled nurses provide sterile dressing changes for surgical wounds, ulcers, injuries, and chronic wounds using advanced dressing products. Medicare accepted.
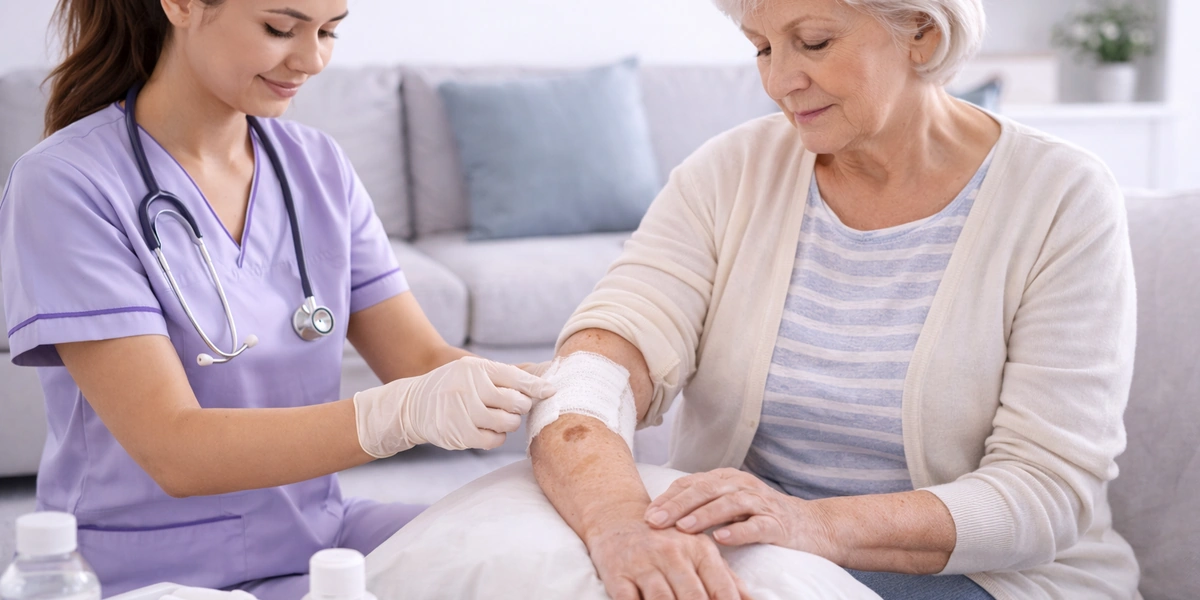
Professional Wound Dressing Services in the Comfort of Your Home
Proper wound dressing is fundamental to healing. The right dressing protects wounds from contamination, maintains optimal moisture levels, manages drainage, and creates conditions that support tissue repair. Yet many wounds require dressing techniques beyond what patients or family members can safely perform at home. At HarvardCare at Home, our skilled nurses provide professional wound dressing changes throughout Los Angeles County, ensuring your wound receives proper care while you remain comfortable at home.
Whether you are recovering from surgery, managing a chronic wound, or dealing with an injury that requires ongoing attention, regular professional dressing changes can mean the difference between smooth healing and complications. Our nurses bring the expertise, supplies, and clinical judgment needed to keep your wound on track toward closure.
Why Professional Dressing Changes Matter
Wound dressing might seem straightforward, but proper technique requires knowledge and skill that comes from professional training and experience.
Preventing Infection
Open wounds are vulnerable to bacterial contamination that can lead to serious infection. Professional dressing changes use sterile technique to minimize contamination risk. Our nurses know how to handle wounds without introducing pathogens, how to recognize early signs of infection, and how to maintain the clean environment wounds need to heal safely.
Optimizing the Healing Environment
Modern wound science has established that wounds heal best in a moist, balanced environment—not too wet, not too dry. Different wounds require different moisture levels, and these needs change as wounds progress through healing stages. Our nurses select dressings that create optimal conditions for your specific wound at each stage of healing.
Monitoring for Problems
Every dressing change is an opportunity for clinical assessment. Our nurses evaluate wound appearance, measure progress, check for signs of infection or complications, and assess surrounding tissue health. This regular monitoring catches problems early when they are easiest to address.
Minimizing Trauma
Improper dressing removal can damage fragile new tissue, setting back healing progress. Our nurses use appropriate techniques and products to remove dressings gently, protecting the wound bed from unnecessary trauma. We also select dressings designed for atraumatic removal when appropriate.
Types of Wounds Requiring Dressing Changes
Our wound dressing services address a wide range of wound types with varying care requirements.
Surgical Wounds
Post-operative incisions need regular dressing changes to protect healing tissue, absorb drainage, and allow monitoring for complications like infection or dehiscence. Surgical wound care follows specific protocols based on procedure type, surgeon preferences, and healing progress. Our nurses are experienced with dressing requirements for orthopedic, abdominal, cardiac, and other surgical procedures.
Traumatic Wounds
Lacerations, abrasions, burns, and other injuries from accidents require professional care during healing. These wounds may have irregular shapes, varying depths, and contamination concerns that need skilled management. We provide dressing changes that protect healing tissue while accommodating the unique characteristics of each traumatic wound.
Ulcers and Chronic Wounds
Diabetic ulcers, venous ulcers, pressure injuries, and other chronic wounds typically require frequent dressing changes as part of a comprehensive treatment plan. These dressing changes are not routine—they involve assessment, debridement when needed, and careful dressing selection based on wound characteristics.
Drain Sites and Tube Exits
Surgical drains, feeding tubes, tracheostomy sites, and other tube exit points require specialized dressing care to prevent infection and skin breakdown. Our nurses are trained in the specific protocols for various drain and tube types.
Skin Tears and Fragile Skin Wounds
Elderly patients with thin, fragile skin are prone to skin tears that require gentle handling and appropriate dressings. Standard bandages and tapes can cause further damage to delicate skin. We use specialized products and techniques designed for fragile skin care.
Understanding Wound Dressings
The world of wound dressings has expanded dramatically, offering options far beyond simple gauze. Understanding the types of dressings helps explain why professional selection matters.
Traditional Gauze Dressings
Gauze remains useful for certain applications—highly draining wounds, wounds requiring packing, and situations where frequent inspection is needed. However, gauze can stick to wound beds, cause pain on removal, and allow wounds to dry out. Our nurses use gauze appropriately while avoiding its pitfalls.
Film Dressings
Transparent adhesive films protect wounds while allowing visual inspection and creating a moist environment. They work well for superficial wounds with minimal drainage, IV sites, and as secondary dressings over other products.
Foam Dressings
Foam dressings absorb moderate to heavy drainage while maintaining moisture balance at the wound surface. They provide cushioning and protection, making them useful for pressure-prone areas. Various foam products address different drainage levels and wound depths.
Hydrocolloid Dressings
These adhesive dressings contain gel-forming agents that absorb drainage and create a moist healing environment. They work well for partial-thickness wounds with light to moderate drainage and can remain in place for several days, reducing dressing change frequency.
Alginate and Hydrofiber Dressings
Derived from seaweed or cellulose, these highly absorbent dressings are ideal for wounds with heavy drainage or those requiring packing. They gel as they absorb fluid, conforming to wound contours and maintaining a moist environment.
Antimicrobial Dressings
Dressings containing silver, honey, iodine, or other antimicrobial agents help manage bacterial burden in colonized or infected wounds. These specialized products are used when infection risk is elevated or bacterial levels need reduction.
Collagen and Matrix Dressings
Advanced dressings containing collagen or other biological materials provide scaffolding for tissue growth and promote healing in stalled wounds. These products are typically reserved for wounds not responding to standard approaches.
Negative Pressure Dressings
Negative pressure wound therapy systems use specialized dressings connected to suction devices. These complex dressings require professional application and management.
Our Dressing Change Process
Professional wound dressing changes follow a systematic approach that ensures safety and promotes healing.
Preparation
Before touching your wound, we gather all necessary supplies, establish a clean work area, and position you comfortably. Proper preparation prevents contamination and ensures the dressing change proceeds smoothly.
Dressing Removal
Old dressings are removed carefully to minimize trauma to healing tissue. When dressings adhere to wound beds, we use saline or other solutions to loosen them gently rather than pulling. We observe the removed dressing for information about drainage amount and character.
Wound Cleansing
Most wounds benefit from gentle cleansing during dressing changes. We use appropriate solutions—typically saline for clean wounds—applied with techniques that remove debris without damaging tissue. Cleansing method and frequency are tailored to wound characteristics and healing stage.
Wound Assessment
With the wound exposed, we perform thorough assessment. We evaluate wound size through measurement and comparison to previous visits. We examine tissue type—granulation, epithelialization, slough, or necrotic tissue. We check wound edges and surrounding skin. We look for signs of infection including increased redness, warmth, swelling, odor, or purulent drainage. This assessment guides dressing selection and identifies any concerns requiring physician notification.
Dressing Application
New dressings are applied using sterile technique. We select the appropriate primary dressing for direct wound contact based on current wound characteristics, then secure it with suitable secondary dressings and tape or wraps. Proper application ensures the dressing stays in place, maintains the intended moisture environment, and does not create pressure or irritation.
Documentation
We document every dressing change thoroughly, recording wound measurements, appearance, drainage, surrounding skin condition, dressings used, and patient response. This documentation tracks healing progress and provides essential information for your healthcare team.
Frequency of Dressing Changes
How often dressings need changing depends on wound type, drainage level, and healing stage.
Daily Dressing Changes
Some wounds require daily dressing changes, particularly those with heavy drainage, active infection, or during early post-surgical healing. Daily changes allow close monitoring and frequent reassessment.
Every Other Day or Three Times Weekly
Many wounds do well with dressing changes every two to three days. This frequency balances monitoring needs with allowing dressings time to work and minimizing wound disturbance.
Extended Wear Dressings
Some modern dressings are designed to remain in place for up to seven days when wound conditions permit. These extended wear products reduce disruption to healing tissue and decrease care burden. We use them when appropriate based on wound assessment.
Adjusting Frequency
Dressing change frequency is not fixed—it adjusts based on wound progress. As drainage decreases and healing advances, we typically reduce frequency. Conversely, problems like increased drainage or infection signs may require more frequent changes temporarily.
What We Bring to Your Home
Our nurses arrive equipped with supplies needed for your dressing change. We maintain clean technique throughout and dispose of used materials safely. For wounds requiring specialized dressings, we coordinate with suppliers to ensure appropriate products are available. You do not need to worry about obtaining wound care supplies—we handle those logistics.
Education and Training
When appropriate and desired, we teach patients and family members to perform dressing changes between nursing visits. This education includes proper hand hygiene and clean technique, step-by-step dressing change procedures, recognition of problems requiring professional attention, and supply management and reordering. Not all wounds are suitable for non-professional care, and we make recommendations based on wound complexity and family capability.
Coordination of Care
We communicate regularly with your physician about wound progress, notifying them promptly of any concerns. When wounds are not progressing as expected, we collaborate with your healthcare team to adjust the treatment plan. For complex wounds, we coordinate with wound care specialists, surgeons, and other providers as needed.
Coverage and Getting Started
Wound dressing changes provided by skilled nurses are covered by Medicare, Medi-Cal, and most insurance plans when medically necessary and ordered by a physician. Our team verifies your coverage and manages authorization so you can focus on healing.
If you have a wound requiring regular dressing changes, contact HarvardCare at Home today. Our skilled nurses are ready to provide professional wound dressing services in your home, giving your wound the expert care it needs to heal properly. Call us for a free consultation and take the first step toward better wound care.
FAQs
Do you have questions?
Got questions about Wound Dressing Changes at Home? Here are answers to what patients and families ask most.
For some wounds, yes. We can teach family members proper technique for dressing changes when appropriate. However, not all wounds are suitable for non-professional care—complex wounds, those requiring sterile technique, or wounds needing clinical assessment at each change should be managed by nurses. We evaluate your specific situation and provide training when it is safe and appropriate to do so.
You do not need to worry about supplies. Our nurses bring all necessary materials for your dressing change including cleansing solutions, appropriate dressings, securing materials, and disposal bags. For ongoing care, we coordinate with medical supply companies to ensure you have needed products. If your wound requires specialized dressings, we arrange for those as well.
Wounds change as they heal, and optimal dressings change with them. Early wounds with heavy drainage need absorbent dressings, while later-stage wounds may benefit from dressings that maintain moisture and promote cell growth. Infection concerns might require antimicrobial dressings temporarily. Your nurse selects dressings based on current wound characteristics at each visit, adjusting as your wound evolves through healing stages.
Contact us for guidance. In many cases, you can apply a clean, dry dressing to protect the wound until your next scheduled visit. If the wound looks concerning—increased redness, swelling, drainage, or odor—let us know immediately as we may need to see you sooner. We provide instructions for managing common situations between visits and are available to answer questions when they arise.
TESTIMONIALS
What Our Patients & Families Say
AREAS WE SERVE
Wound Dressing Change at Home Near You
Our licensed healthcare professionals provide wound dressing changes at home with careful, sterile technique - so you can recover comfortably without repeated clinic visits. We serve patients and families across Los Angeles County.
- A
- Agoura Hills
- Alhambra
- Altadena
- Arcadia
- B
- Bel Air
- Bellflower
- Beverly Hills
- Boyle Heights
- Brentwood
- Burbank
- C
- Calabasas
- Carson
- Century City
- Cerritos
- Claremont
- Compton
- Covina
- Culver City
- D
- Diamond Bar
- Downey
- E
- Eagle Rock
- East Los Angeles
- Echo Park
- Encino
- G
- Gardena
- Glendale
- Glendora
- Granada Hills
- H
- Hacienda Heights
- Hancock Park
- Harbor City
- Hawthorne
- Highland Park
- Hollywood
- Hollywood Hills
- I
- Inglewood
- K
- Koreatown
- L
- La Crescenta-Montrose
- La Mirada
- Lakewood
- Lincoln Heights
- Long Beach
- Los Angeles
- Los Feliz
- M
- Malibu
- Manhattan Beach
- Mar Vista
- Marina del Rey
- Mid-City
- Mid-Wilshire
- Miracle Mile
- Monrovia
- Montebello
- Monterey Park
- N
- North Hollywood
- Northridge
- Norwalk
- P
- Pacific Palisades
- Palms
- Palos Verdes Estates
- Palos Verdes Peninsula
- Panorama City
- Pasadena
- Pico Rivera
- Playa Vista
- Pomona
- Porter Ranch
- R
- Rancho Palos Verdes
- Redondo Beach
- Reseda
- Rolling Hills Estates
- Rowland Heights
- S
- San Dimas
- San Gabriel
- San Marino
- San Pedro
- Santa Clarita
- Santa Monica
- Sawtelle
- Sherman Oaks
- Silver Lake
- South Gate
- South Pasadena
- Studio City
- T
- Tarzana
- Torrance
- V
- Van Nuys
- Venice
- W
- West Covina
- West Hollywood
- West Los Angeles
- Westchester
- Westlake Village
- Westwood
- Whittier
- Wilmington
- Woodland Hills
More Services
In-Home Wound Care Services
- Board-certified wound care nurses
- Personalized treatment plans
- All wound types treated
Diabetic Wound Care at Home
- Diabetes wound specialists
- Blood sugar optimization support
- Advanced offloading techniques
Skilled Nursing Care at Home
- Registered nurses available 7 days a week
- Comprehensive care coordination
- IV therapy and infusion services
 HarvardCare at Home
HarvardCare at Home