A wound is considered non-healing (or chronic) when it has not shown meaningful improvement within 30 days of appropriate treatment, or has remained open for 6 weeks or longer. Non-healing wounds often stall because of underlying factors like poor circulation, infection, malnutrition, or uncontrolled diabetes. Any wound that is getting larger, more painful, or showing signs of infection instead of improving should be evaluated by a wound care specialist as soon as possible.
WOUND CARE
Non-Healing Wound Care at Home
Struggling with a wound that won't heal? HarvardCare at Home provides expert non-healing wound care in Los Angeles County. Advanced treatments, certified nurses, real results. Medicare accepted. Call for a free consultation today!
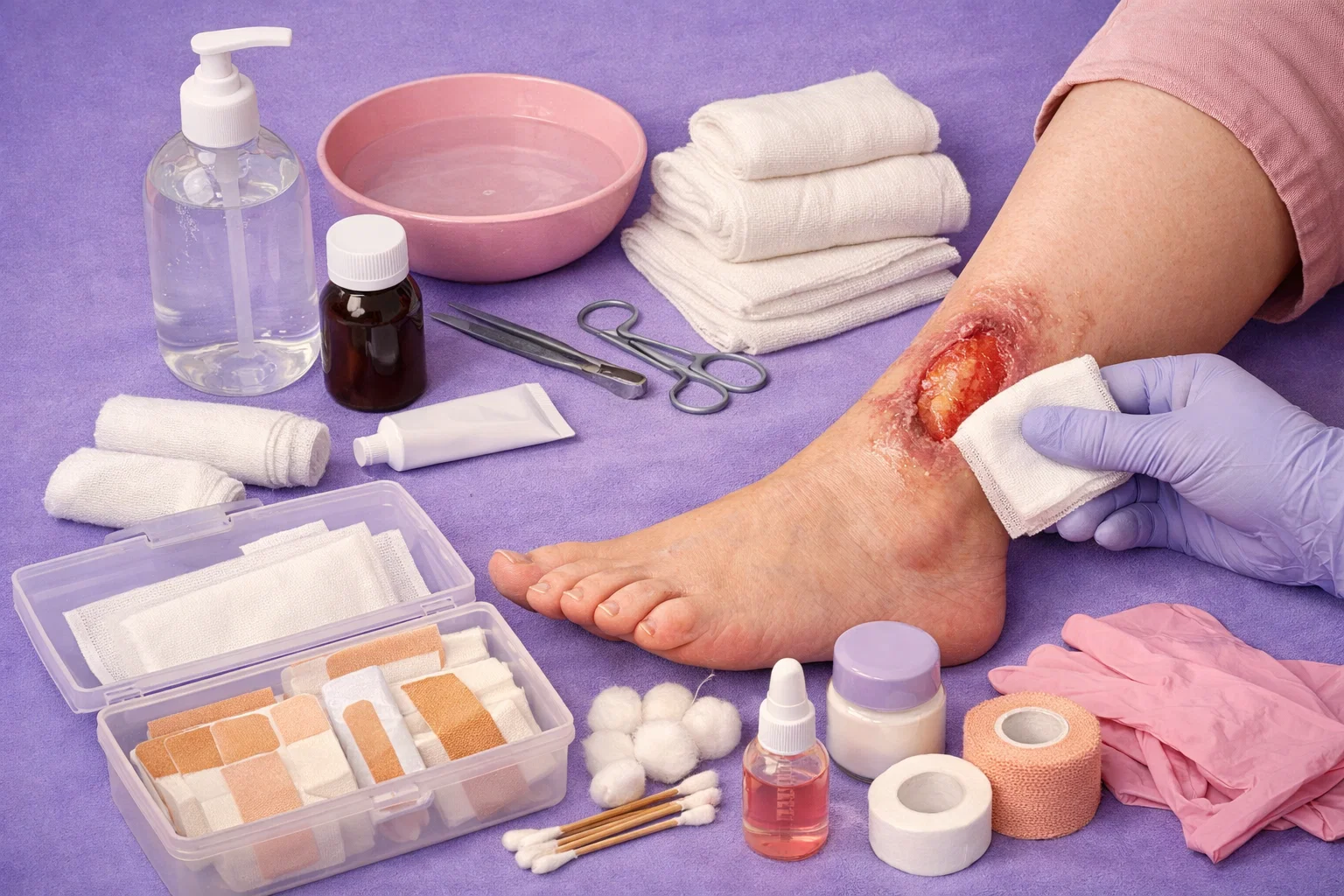
Why Won’t My Wound Heal? Expert Treatment for Stubborn, Non-Healing Wounds at Home
A wound that refuses to heal is more than frustrating—it is a medical concern that demands professional attention. If you have a wound that has not shown meaningful progress in 30 days or has persisted for weeks or months despite treatment, you are dealing with a non-healing wound (also called a chronic wound or stalled wound). Left untreated, these wounds can lead to dangerous infections, tissue death, hospitalization, and even amputation.
At HarvardCare at Home, our certified wound care specialists treat non-healing wounds throughout Los Angeles County—right in your home. We do not just change dressings. We identify why your wound stopped healing, eliminate the barriers to recovery, and apply advanced treatments that restart the healing process. Medicare, Medi-Cal, and most private insurance accepted.
What Is a Non-Healing Wound?
A non-healing wound is any wound that fails to progress through normal healing stages within an expected timeframe. In medical terms, a wound is considered chronic or non-healing when it:
- Has not improved in 30 days despite appropriate care
- Remains open for 6 weeks or longer
- Keeps reopening after partial healing
- Gets larger instead of smaller
- Shows signs of infection that do not resolve
Non-healing wounds are far more common than most people realize. An estimated 6.5 million Americans suffer from chronic wounds, and that number is growing as the population ages and chronic conditions like diabetes become more prevalent.
Common Types of Non-Healing Wounds
Almost any wound can become chronic, but certain types are especially prone to stalling:
- Diabetic foot ulcers — caused by nerve damage and poor circulation from diabetes
- Venous leg ulcers — resulting from faulty valves in leg veins
- Arterial ulcers — caused by inadequate blood supply to the extremities
- Pressure ulcers (bedsores) — from sustained pressure on skin over bony areas
- Surgical wounds — incisions that dehisce (open) or fail to close properly
- Traumatic wounds — injuries from accidents that stall during healing
- Radiation wounds — tissue damage from cancer radiation therapy
Regardless of wound type, the underlying principle is the same: something is blocking your body’s natural healing process, and identifying that barrier is the key to getting your wound to close.
Why Wounds Stop Healing: The 7 Most Common Causes
Understanding why your wound stalled is the first step toward fixing it. Here are the most common reasons wounds fail to heal:
1. Poor Blood Circulation
Your blood delivers oxygen, nutrients, and immune cells to the wound site. When circulation is compromised—from peripheral arterial disease, diabetes, or vascular conditions—your body simply cannot supply what the wound needs to repair itself.
2. Uncontrolled Diabetes
High blood sugar damages blood vessels, impairs white blood cell function, and disrupts every phase of wound healing. Diabetic patients with an A1C above 7% face significantly slower healing and higher infection risk.
3. Infection
Bacteria in the wound consume resources meant for healing, produce toxins that destroy tissue, and trigger excessive inflammation. Chronic wounds often harbor biofilm—organized bacterial colonies that resist antibiotics and create a persistent barrier to healing.
4. Inadequate Nutrition
Wound healing is an energy-intensive process. Your body needs:
- Protein — the primary building block for new tissue
- Vitamin C — essential for collagen formation
- Zinc — critical for cell division and immune function
- Adequate calories — to fuel the repair process
Malnourished patients often see immediate improvement once nutritional deficiencies are addressed.
5. Continued Pressure or Trauma
Wounds cannot heal if the force that caused them continues. Pressure ulcers need pressure relief. Diabetic foot ulcers need offloading. Venous ulcers need compression. Without removing the underlying mechanical cause, no amount of wound care will succeed.
6. Medications That Impair Healing
Certain medications actively slow healing, including corticosteroids, immunosuppressants, some chemotherapy drugs, and anticoagulants. Your wound care nurse reviews your medication list and coordinates with your physician when medication adjustments could support healing.
7. Dead Tissue in the Wound Bed
Necrotic (dead) tissue, slough, and biofilm create a physical and biological barrier to healing. The wound cannot generate new tissue until this debris is removed through debridement—a critical step many patients have never received.
How We Treat Non-Healing Wounds at Home
Our treatment goes far beyond basic wound care. We use a systematic, evidence-based approach designed to identify barriers, eliminate them, and restart healing.
Step 1: Comprehensive Wound Assessment
At your first visit, our wound care nurse conducts a detailed evaluation including:
- Complete wound measurement — length, width, depth, undermining, tunneling
- Wound bed assessment — tissue types present (granulation, slough, eschar, necrotic)
- Drainage analysis — amount, color, consistency, odor
- Surrounding skin evaluation — redness, swelling, maceration, callus
- Vascular assessment — perfusion status, pulse checks, sensation testing
- Medical history review — conditions, medications, nutrition, prior treatments
- Photo documentation — for objective progress tracking
This thorough assessment reveals why your wound is not healing and guides a targeted treatment plan.
Step 2: Wound Bed Preparation
Before a wound can heal, it must be prepared. Our wound bed preparation protocol includes:
- Debridement — removing dead tissue, slough, and biofilm using sharp, autolytic, or enzymatic methods
- Bacterial management — addressing infection and biofilm to reduce bacterial burden
- Moisture balance — correcting wounds that are too wet or too dry
- Edge advancement — stimulating wound edges that have become dormant and stopped migrating
This approach, known in wound care as the TIME framework (Tissue, Infection/Inflammation, Moisture, Edge), is the gold standard for chronic wound management.
Step 3: Advanced Wound Therapies
Non-healing wounds often require treatments beyond conventional dressings. We offer:
- Negative pressure wound therapy (Wound VAC) — accelerates granulation and removes excess fluid
- Antimicrobial dressings — silver, honey, and iodine-based options that combat biofilm
- Collagen dressings — provide a scaffold for new tissue growth
- Growth factor therapies — stimulate cellular repair mechanisms
- Compression therapy — essential for venous insufficiency wounds
- Offloading devices — redistribute pressure away from diabetic foot ulcers
We select therapies based on your wound’s specific characteristics and adjust as your wound responds.
Step 4: Treating the Whole Patient
A wound does not exist in isolation. To heal your wound, we often need to address:
- Blood sugar control — coordinating with your physician for tighter diabetes management
- Nutrition optimization — assessing deficiencies and recommending supplementation
- Medication review — identifying drugs that may impair healing
- Circulation support — compression, elevation, and activity recommendations
- Smoking cessation — nicotine severely restricts blood flow to wounds
Step 5: Ongoing Monitoring and Adjustment
We track your wound’s progress at every visit using standardized measurements and photography. If a wound is not responding as expected, we do not simply continue the same approach—we reassess, investigate, and adjust. This proactive monitoring ensures your treatment evolves with your wound.
Warning Signs: When to Seek Help for a Non-Healing Wound
Contact a wound care professional immediately if you notice:
- A wound that has not improved in 2-4 weeks
- Increasing pain, redness, warmth, or swelling around the wound
- Foul-smelling or discolored drainage
- Wound getting larger despite treatment
- Fever or chills accompanying a wound
- Black or dark tissue in the wound bed
- Exposed bone, tendon, or muscle
Do not wait. The longer a non-healing wound persists, the harder it becomes to treat and the greater the risk of serious complications.
Why Home-Based Treatment Gets Better Results
Treating non-healing wounds at home is not just convenient—it is clinically superior in several ways:
- Lower infection risk — your home has fewer resistant bacteria than hospitals and clinics
- Better compliance — eliminating travel barriers means you receive every scheduled treatment
- Real-world assessment — we see the actual conditions affecting your wound (shoes, surfaces, equipment)
- Caregiver training — family members learn wound care techniques specific to your situation
- Comfort and healing — reduced stress and better rest support faster recovery
- Consistent monitoring — regular visits catch complications before they become emergencies
Who Qualifies for Home Wound Care?
You may qualify for home wound care services if:
- You have a non-healing wound requiring skilled nursing care
- You are considered homebound (leaving home is difficult or medically inadvisable)
- Your physician orders home health wound care services
- You have Medicare, Medi-Cal, or qualifying private insurance
Not sure if you qualify? Call us for a free eligibility check — our team handles all insurance verification and physician coordination.
Insurance Coverage for Non-Healing Wound Care
Skilled wound care for non-healing wounds is covered by Medicare Part A for homebound patients with a physician’s order. This includes:
- Wound assessment and skilled nursing visits
- Dressing changes and wound treatments
- Debridement and wound bed preparation
- Advanced therapies like negative pressure wound therapy
- Patient and caregiver education
Medi-Cal and most private insurance provide similar coverage. Our team handles all authorization and paperwork.
Take the First Step Toward Healing
A wound that will not heal is not something to live with—it is something to treat. Every day a non-healing wound remains open increases the risk of infection, complications, and declining health.
HarvardCare at Home provides expert non-healing wound care throughout Los Angeles County. Our certified wound care nurses have the training, technology, and experience to heal wounds that others have not been able to close.
Call today for a free consultation. Let us assess your wound, explain your treatment options, and start you on the path to healing. Do not let another day pass with a wound that is not getting better.
FAQs
Do you have questions?
Got questions about Non-Healing Wound Care at Home? Here are answers to what patients and families ask most.
The most common reasons wounds fail to heal despite treatment include undiagnosed or uncontrolled diabetes affecting blood supply and immune function, biofilm (organized bacterial colonies) hiding in the wound bed that resist standard antibiotics, inadequate debridement leaving dead tissue that blocks healing, poor nutrition depriving your body of building blocks for repair, medications that suppress healing like steroids or immunosuppressants, and insufficient treatment of the underlying cause such as lack of compression for venous ulcers. Our specialists identify the specific barriers affecting your wound and eliminate them.
Yes—even long-standing chronic wounds can heal with the right treatment approach. The key is identifying and correcting the factors that have been preventing healing. Many patients come to us after months or years of unsuccessful treatment elsewhere, and their wounds respond once we address underlying issues like biofilm, nutritional deficiencies, or inadequate circulation management. While older wounds may take longer to close, healing is possible for most patients with comprehensive evidence-based care.
We offer multiple advanced therapies based on your wound's specific needs, including negative pressure wound therapy (Wound VAC) that accelerates tissue growth, specialized debridement techniques to remove dead tissue and biofilm, antimicrobial dressings containing silver, medical-grade honey, or iodine, collagen-based dressings that provide scaffolding for new tissue, compression therapy for venous insufficiency wounds, and growth factor therapies that stimulate cellular repair. Treatment selection is based on thorough wound assessment and adjusted as your wound responds.
Visit frequency is based on wound severity and treatment needs. Complex non-healing wounds typically require visits 2-3 times per week initially, especially if debridement, VAC therapy, or intensive monitoring is needed. As healing progresses and the wound stabilizes, visits may decrease to once or twice weekly. We adjust the schedule based on your wound's response—our goal is providing the care intensity your wound needs at every stage of healing.
Yes, skilled nursing wound care for non-healing wounds is covered by Medicare Part A for homebound patients with a physician's order. Coverage includes nursing visits, wound assessments, dressing changes, debridement, advanced therapies like wound VAC, and patient education. Medi-Cal and most private insurance plans provide similar coverage. We handle all insurance verification, authorization, and paperwork so you can focus entirely on healing.
Supporting your wound care between nursing visits makes a significant difference. Keep blood sugar well-controlled if you are diabetic—this is the single most important thing diabetic patients can do. Eat adequate protein and take any recommended supplements. Follow all activity and positioning instructions. Keep the wound clean and protected. Do not smoke, as nicotine severely restricts blood flow needed for healing. Attend all follow-up visits and report any changes or concerns promptly.
Seek professional help immediately if your wound has not improved in 2-4 weeks, is getting larger instead of smaller, produces foul-smelling or discolored drainage, has increasing redness spreading outward, is more painful than before, shows black or dark tissue, exposes bone or tendon, or is accompanied by fever. Early intervention prevents minor wound problems from becoming serious medical emergencies. Do not wait for a wound to become dangerous before getting expert help.
Home wound care provides several advantages over clinic-based treatment. You receive care in a lower-infection-risk environment. There is no painful or difficult travel with open wounds. Your nurse assesses real-world factors affecting your wound—your bed, shoes, surfaces, and equipment. Family caregivers receive hands-on training in your actual home. And consistent scheduling without transportation barriers means you never miss treatments. Many patients who struggled to heal at wound clinics see breakthroughs with home-based care because of improved treatment consistency.
During your first visit, your wound care nurse performs a comprehensive assessment. This includes detailed wound measurement and photography, wound bed tissue analysis, drainage evaluation, surrounding skin assessment, vascular and sensation testing, review of your complete medical history and medications, nutritional screening, and discussion of all previous treatments. Based on this evaluation, we develop a targeted treatment plan addressing the specific barriers preventing your wound from healing. You will understand exactly why your wound has stalled and what we are going to do about it.
TESTIMONIALS
What Our Patients & Families Say
AREAS WE SERVE
Non-Healing Wound Care at Home Near You
Our licensed healthcare professionals provide expert care in the comfort of your home. We proudly serve patients and families throughout Los Angeles County.
- A
- Agoura Hills
- Alhambra
- Altadena
- Arcadia
- B
- Bel Air
- Bellflower
- Beverly Hills
- Boyle Heights
- Brentwood
- Burbank
- C
- Calabasas
- Carson
- Century City
- Cerritos
- Claremont
- Compton
- Covina
- Culver City
- D
- Diamond Bar
- Downey
- E
- Eagle Rock
- East Los Angeles
- Echo Park
- Encino
- G
- Gardena
- Glendale
- Glendora
- Granada Hills
- H
- Hacienda Heights
- Hancock Park
- Harbor City
- Hawthorne
- Highland Park
- Hollywood
- Hollywood Hills
- I
- Inglewood
- K
- Koreatown
- L
- La Crescenta-Montrose
- La Mirada
- Lakewood
- Lincoln Heights
- Long Beach
- Los Angeles
- Los Feliz
- M
- Malibu
- Manhattan Beach
- Mar Vista
- Marina del Rey
- Mid-City
- Mid-Wilshire
- Miracle Mile
- Monrovia
- Montebello
- Monterey Park
- N
- North Hollywood
- Northridge
- Norwalk
- P
- Pacific Palisades
- Palms
- Palos Verdes Estates
- Palos Verdes Peninsula
- Panorama City
- Pasadena
- Pico Rivera
- Playa Vista
- Pomona
- Porter Ranch
- R
- Rancho Palos Verdes
- Redondo Beach
- Reseda
- Rolling Hills Estates
- Rowland Heights
- S
- San Dimas
- San Gabriel
- San Marino
- San Pedro
- Santa Clarita
- Santa Monica
- Sawtelle
- Sherman Oaks
- Silver Lake
- South Gate
- South Pasadena
- Studio City
- T
- Tarzana
- Torrance
- V
- Van Nuys
- Venice
- W
- West Covina
- West Hollywood
- West Los Angeles
- Westchester
- Westlake Village
- Westwood
- Whittier
- Wilmington
- Woodland Hills
More Services
In-Home Wound Care Services
- Board-certified wound care nurses
- Personalized treatment plans
- All wound types treated
Diabetic Wound Care at Home
- Diabetes wound specialists
- Blood sugar optimization support
- Advanced offloading techniques
Skilled Nursing Care at Home
- Registered nurses available 7 days a week
- Comprehensive care coordination
- IV therapy and infusion services
 HarvardCare at Home
HarvardCare at Home