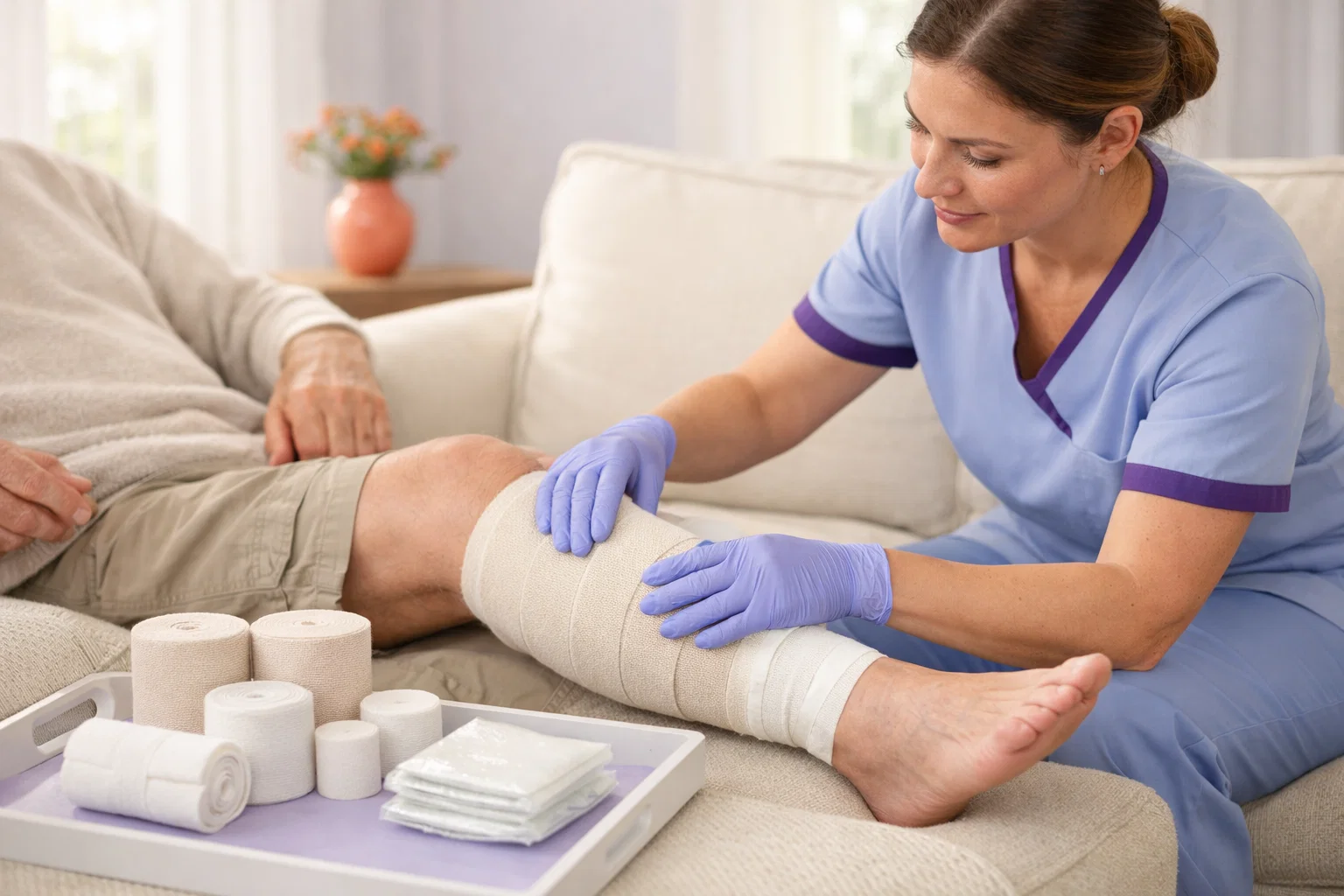
Understanding Compression Therapy
Compression therapy is a cornerstone treatment for many types of leg wounds and circulation problems. By applying controlled external pressure to the legs, compression supports healing for venous ulcers, reduces swelling, and improves overall leg health. Understanding how compression works and why it is so important helps patients appreciate this essential treatment and comply with recommendations.
While compression may seem like a simple concept, therapeutic compression for wound healing requires professional assessment, proper application, and ongoing monitoring. When used appropriately, compression dramatically improves healing outcomes for suitable patients.
How Compression Therapy Works
Compression therapy applies external pressure to the leg, counteracting forces that contribute to tissue damage and impaired healing.
Supporting Venous Return
Leg veins carry blood back to the heart against gravity. Damaged vein valves allow blood to flow backward, pooling in the lower legs. This venous insufficiency causes increased pressure in leg veins.
External compression supports weakened veins, helping them function more effectively. Blood moves upward more efficiently, reducing the venous pressure that damages tissue.
Reducing Edema
Swelling (edema) occurs when fluid leaks from blood vessels into surrounding tissue. Chronic swelling stretches skin, impairs oxygen delivery, and creates conditions promoting wound development.
Compression prevents fluid accumulation and helps move existing edema out of the legs. Reduced swelling improves tissue health and wound healing.
Improving Circulation
By supporting venous return and reducing edema, compression improves overall circulation in the legs. Better blood flow delivers oxygen and nutrients to healing tissue while removing waste products.
Creating Healing Conditions
The combined effects of compression, including reduced venous pressure, decreased swelling, and improved circulation, create conditions that allow wounds to heal. Without compression, venous ulcers and other circulation-related wounds cannot heal effectively regardless of what treatments are applied to the wound itself.
Conditions Treated with Compression
Compression therapy benefits several conditions affecting the legs.
Venous Leg Ulcers
Compression is the primary treatment for venous ulcers. These wounds result from chronic venous insufficiency and cannot heal without addressing the underlying circulation problem. Compression provides that essential treatment.
Research consistently demonstrates that venous ulcers treated with compression heal faster and more completely than those treated without compression.
Chronic Venous Insufficiency
Even before ulcers develop, compression treats venous insufficiency, reducing symptoms and preventing progression to ulceration.
Lymphedema
Compression helps manage lymphedema, a condition of chronic swelling due to lymphatic system problems. Specialized compression techniques address lymphatic drainage.
Post-Thrombotic Syndrome
After deep vein thrombosis (blood clots), compression helps prevent and manage the chronic symptoms that can develop.
Edema from Various Causes
Compression may benefit edema from heart failure, kidney disease, or other conditions, though treatment must be coordinated with management of the underlying condition.
Types of Compression
Different compression methods serve different purposes and patient needs.
Compression Bandages
Multi-layer compression bandages are commonly used for active venous ulcer treatment. These systems typically include multiple layers that work together to provide therapeutic pressure.
Short-Stretch Bandages
Short-stretch bandages provide high working pressure during activity and lower resting pressure. They require professional application but are effective for venous ulcer treatment.
Long-Stretch Bandages
Long-stretch (elastic) bandages maintain more consistent pressure but may be less comfortable and have higher resting pressure. They are more commonly used in acute care settings.
Multi-Component Systems
Multi-layer systems combine different materials to achieve desired pressure and comfort. These systems are widely used for venous ulcer treatment.
Compression Stockings
Compression stockings are elastic garments that apply graduated pressure, highest at the ankle and decreasing up the leg. They are used for maintenance after ulcer healing, prevention of ulcer recurrence, management of chronic venous insufficiency, and prevention of swelling during prolonged standing or sitting.
Stockings come in different compression levels measured in millimeters of mercury (mmHg). Higher pressure provides more support but may be harder to apply. Professional fitting ensures appropriate sizing and pressure.
Compression Wraps
Adjustable compression wraps allow patients to apply and remove compression themselves. These devices may be useful when stockings are too difficult to apply or for patients needing adjustable compression.
Pneumatic Compression
Pneumatic compression devices use inflatable chambers that sequentially compress the leg. These devices may benefit patients who cannot tolerate constant compression or who need additional treatment beyond bandages or stockings.
Why Professional Assessment Matters
Compression therapy requires professional assessment before beginning treatment.
Ruling Out Arterial Disease
Compression is contraindicated or must be modified for patients with significant arterial disease. Applying compression to legs with inadequate arterial blood flow can cause serious harm including tissue death.
Before compression therapy, clinicians assess arterial circulation, typically using the ankle-brachial index (ABI). This simple test compares blood pressure at the ankle to arm blood pressure, identifying arterial problems that affect compression safety.
Determining Appropriate Pressure
Therapeutic compression for venous ulcers requires specific pressure levels. Too little pressure is ineffective. Too much pressure can cause problems, particularly for patients with some arterial compromise. Professional assessment determines safe, effective pressure for each patient.
Selecting Appropriate Method
Different compression methods suit different situations. Multi-layer bandages are appropriate for active ulcer treatment. Stockings work for maintenance and prevention. Wraps may be needed for patients who cannot manage stockings. Professional assessment guides method selection.
Professional Wound Care with Compression
For patients with venous ulcers, wound care and compression therapy go together.
Combined Treatment
Professional wound care addresses the ulcer through assessment, debridement, and appropriate dressings. Compression addresses the underlying circulation problem that caused the ulcer and prevents healing without treatment.
Neither treatment alone is sufficient. Wound care without compression rarely heals venous ulcers. Compression alone does not address wound bed issues that require professional management.
Home Health Compression
Skilled nursing through home health services can provide compression bandage application along with wound care. This combined service delivers comprehensive venous ulcer treatment at home.
Education and Training
Home health clinicians educate patients and caregivers about compression importance, what to watch for between visits, and how to manage compression stockings when appropriate.
Living with Compression Therapy
Compression therapy is often a long-term or lifelong commitment for patients with venous disease.
During Active Treatment
While treating a venous ulcer with compression bandages, patients should keep bandages dry and intact between changes, elevate legs when resting, report problems like increased pain, numbness, or color changes, stay active with walking as tolerated, and attend all scheduled wound care visits.
Long-Term Compression
After ulcer healing, continued compression stocking use prevents recurrence. This typically means wearing stockings during waking hours every day, replacing stockings when they lose elasticity (usually every three to six months), putting stockings on first thing in the morning before swelling develops, and removing stockings at bedtime.
Compliance Challenges
Compression stockings can be difficult to apply, especially for patients with limited hand strength, flexibility, or vision. Strategies to improve compliance include using donning aids designed to help apply stockings, trying different stocking styles to find the most comfortable option, considering compression wraps if stockings are too difficult, and involving family caregivers in stocking application.
When to Contact Providers
Contact your healthcare provider if compression causes increased pain or discomfort, you notice color changes, numbness, or tingling, skin problems develop under compression, or you cannot apply or tolerate compression.
The Importance of Compression Compliance
Compression only works when used consistently. Studies show that patients who wear compression as prescribed have much better outcomes than those with poor compliance.
Consequences of Non-Compliance
Without consistent compression, venous ulcers heal slowly or not at all, healed ulcers frequently recur, symptoms of venous insufficiency persist, and leg health continues to deteriorate.
Improving Compliance
Understanding why compression matters motivates compliance. Remember that compression treats the underlying problem that caused your wound or symptoms. Wound healing cannot occur without addressing circulation. Continued compression after healing prevents the recurring cycle of ulceration that affects many patients.
If compression is difficult, discuss options with your healthcare provider. Alternative methods or assistance strategies may make compliance achievable.
Compression as Part of Comprehensive Care
Compression therapy is powerful but works best as part of comprehensive care including professional wound management for open wounds, treatment of underlying vein problems when appropriate, lifestyle modifications including activity, elevation, and weight management, skin care to prevent new wounds, and regular monitoring of leg health.
This comprehensive approach addresses venous disease from multiple angles, producing better outcomes than any single treatment alone.
Getting Started with Compression Therapy
If you have a leg wound that is not healing, chronic leg swelling, or symptoms of venous insufficiency, professional evaluation can determine whether compression therapy would benefit you.
Start by discussing symptoms with your healthcare provider. They can assess your circulation, determine whether compression is appropriate, and refer you to wound care or vascular specialists if needed.
For patients with venous ulcers, home health wound care provides professional compression bandaging along with comprehensive wound management, bringing this essential treatment to your home.
 HarvardCare at Home
HarvardCare at Home