Understanding Negative Pressure Wound Therapy
When wounds fail to heal with conventional treatment, advanced therapies can make the difference between prolonged suffering and successful recovery. Wound vac therapy, also called negative pressure wound therapy or NPWT, represents one of the most significant advances in wound care over the past several decades.
Once available only in hospitals, wound vac therapy is now commonly provided at home. This comprehensive guide explains how wound vac therapy works, who benefits from it, and what to expect when receiving this treatment at home.
What Is Wound Vac Therapy?
Wound vac therapy uses controlled negative pressure (suction) to promote wound healing. A specialized dressing covers the wound, connected to a portable pump that continuously or intermittently removes fluid and creates a sealed healing environment.
How It Works
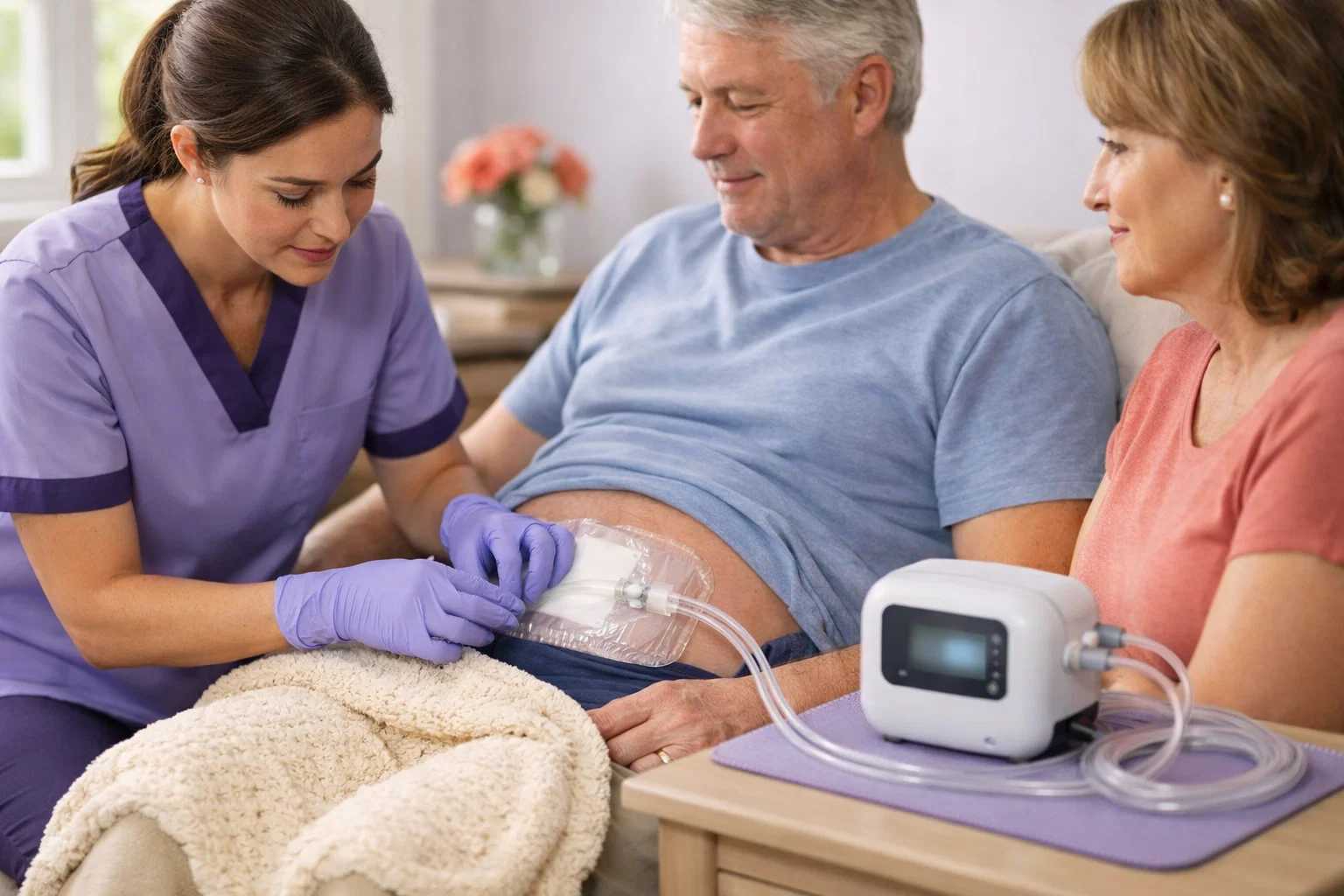
The wound vac system includes several components. A foam or gauze dressing is cut to fit inside the wound. An adhesive drape seals the dressing and wound from outside air. Tubing connects the dressing to the therapy unit. A portable pump creates negative pressure and collects wound fluid in a canister.
When activated, the pump creates suction that removes excess fluid and infectious material, brings wound edges closer together, increases blood flow to the wound bed, stimulates formation of granulation tissue, and reduces bacterial colonization.
Why It Accelerates Healing
Research shows wound vac therapy can significantly speed healing for appropriate wounds. The negative pressure environment triggers biological responses at the cellular level. Blood vessel growth increases. Cell proliferation accelerates. The wound bed transforms more quickly into healthy tissue ready for closure.
Who Benefits from Wound Vac Therapy?
Wound vac therapy is not appropriate for every wound, but for the right wounds, it can be transformative.
Wounds That Respond Well
Wound vac therapy at home is commonly used for chronic wounds that have failed other treatments, diabetic foot ulcers, pressure ulcers stages 3 and 4, venous leg ulcers, dehisced surgical wounds where the incision has opened, traumatic wounds with tissue loss, and wounds with heavy drainage.
If your wound has not improved despite consistent wound dressing changes, wound vac therapy may be the next step.
Conditions Where Wound Vac May Help
Patients with certain conditions often benefit particularly from wound vac therapy including diabetes with foot ulcers, poor circulation affecting healing, surgical complications with wound opening, obesity making wound healing difficult, and multiple failed treatment attempts.
When Wound Vac Is Not Appropriate
Wound vac therapy is not used for wounds with untreated infection requiring antibiotics first, wounds with exposed arteries, veins, or organs, malignant wounds in the treatment area, patients with active bleeding disorders, and wounds with necrotic tissue that has not been debrided.
Your wound care provider evaluates whether wound vac therapy is appropriate for your specific situation.
Getting Started with Home Wound Vac Therapy
Transitioning to wound vac therapy at home involves careful planning and education.
The Evaluation Process
Before starting wound vac therapy, a wound care nurse thoroughly evaluates your wound to confirm wound vac is appropriate, determine optimal settings, assess your home environment, and plan for equipment and supplies.
Physician Orders
Wound vac therapy requires a physician order specifying the type of therapy and settings, dressing change frequency, duration of treatment, and any special instructions.
Equipment Delivery
The wound vac equipment arrives at your home before therapy begins. A representative explains the equipment, demonstrates operation, and ensures you understand basic troubleshooting.
Initial Dressing Application
A trained clinician applies the first wound vac dressing. This initial visit includes thorough wound assessment and measurement, proper foam or gauze dressing placement, secure drape application, connection to the therapy unit, verification that the system is working properly, and education about what to expect.
What to Expect During Treatment
Understanding the day-to-day reality of wound vac therapy helps you prepare for success.
Wearing the Device
The wound vac unit is portable, typically about the size of a small purse. You can carry it with a shoulder strap, place it on a table nearby, or use a belt clip depending on the model.
You will wear the device continuously, usually 22 to 23 hours per day. Brief disconnection for bathing is typically allowed. The therapy works best with minimal interruption.
Sensation During Therapy
When therapy starts, you may feel a pulling or tugging sensation as negative pressure engages. Most patients adjust to this sensation quickly. Some describe mild discomfort initially that resolves within the first day or two. Pain should be manageable and decrease over time.
If you experience significant pain, notify your care team. Adjustments to settings or dressing technique can often improve comfort.
Dressing Changes
Wound vac dressings are changed regularly, typically every 48 to 72 hours. A wound care nurse visits your home to remove the old dressing, assess the wound and document progress, clean the wound appropriately, apply a fresh dressing, and reconnect the system.
Some patients or caregivers learn to perform dressing changes between nursing visits, though professional oversight remains important.
Alarms and Alerts
The wound vac unit has alarms that indicate when attention is needed. Common alerts signal low battery requiring charging, canister full and needing replacement, leak in the seal requiring dressing adjustment, and blockage in the tubing. Your care team teaches you how to respond to each alarm.
Living with a Wound Vac
Wound vac therapy requires adjustments to daily life, but most patients manage well.
Sleep
Many patients worry about sleeping with a wound vac. Most adapt within a few nights. Place the unit on your nightstand or bed. Position tubing to avoid kinking. Use pillows for comfortable positioning. The quiet hum of the pump becomes background noise.
Bathing
You cannot submerge the wound vac dressing in water. Depending on wound location, you may be able to shower with the wound covered and protected, take sponge baths avoiding the dressing area, or briefly disconnect for quick showers with physician approval.
Your care team provides specific bathing instructions based on your wound location and dressing type.
Activity
Activity levels vary based on your wound location and overall health. Many patients remain active during wound vac therapy. The portable unit allows movement around the home. Some patients return to work with their wound vac. Discuss activity guidelines with your care team.
Clothing
Choose loose, comfortable clothing that accommodates the dressing and tubing. Button-front or zip-front tops are often easier than pullovers. Loose pants or skirts work well for lower extremity wounds.
Monitoring Progress
Tracking wound improvement helps you and your care team assess treatment effectiveness.
Signs of Improvement
Positive signs during wound vac therapy include wound getting smaller over time, healthy red granulation tissue forming, drainage decreasing, wound bed filling in, and wound edges contracting inward.
Documentation
Your wound care nurse measures and documents the wound at each visit. Photos may be taken to track visual changes. This documentation demonstrates progress and supports continued insurance coverage.
How Long Treatment Takes
Duration varies significantly based on wound size, location, and your overall health. Some wounds heal within a few weeks. Complex wounds may require months of therapy. Your care team provides estimates based on your specific situation and adjusts as healing progresses.
Potential Complications
While wound vac therapy is generally safe, understanding potential complications helps you recognize problems early.
Bleeding
Some oozing at dressing changes is normal. Significant bleeding requires immediate attention. If blood fills the canister rapidly, disconnect the unit and apply pressure. Contact your care team or seek emergency care.
Infection
Signs of wound infection include increased pain, redness spreading from wound edges, fever, foul odor, and changes in drainage color. Report these symptoms promptly. Infection may require antibiotics and potentially temporary discontinuation of wound vac therapy. Learn more about signs of wound infection.
Skin Problems
The adhesive drape can irritate surrounding skin. Options to address this include different drape products, skin protectant application, and careful drape removal technique.
Pain
Pain should be manageable. Uncontrolled pain warrants evaluation. Possible causes include dressing too tight, foam touching wound edges, or underlying problems requiring assessment.
Transitioning Off Wound Vac
The goal of wound vac therapy is healing to the point where simpler treatment can take over.
Signs You May Be Ready
Transition from wound vac often occurs when the wound has filled with healthy granulation tissue, wound size has decreased significantly, drainage has reduced to manageable levels, and the wound can be managed with conventional dressings.
Next Steps
After wound vac therapy, you may transition to regular wound dressing changes, continue healing with appropriate dressings, proceed to surgical closure if planned, or continue ongoing wound care as needed.
Insurance Coverage
Wound vac therapy is typically covered by Medicare and most insurance plans when medically necessary.
Medicare Coverage
Medicare covers wound vac therapy for qualified patients. You must meet criteria for home health coverage. The wound must be appropriate for negative pressure therapy. Coverage includes the equipment, supplies, and nursing visits for dressing changes. Read our complete guide on Medicare home health coverage.
Private Insurance
Most private insurers cover wound vac therapy with proper documentation of medical necessity. Your home health agency handles prior authorization and documentation requirements.
Finding Wound Vac Therapy in Los Angeles
If you need wound vac therapy in the Los Angeles area, services are available throughout the region. Professional home wound care reaches communities including Beverly Hills, Santa Monica, Pasadena, Torrance, Glendale, and surrounding areas.
For wound care in specific locations, visit our service area pages like wound care in Beverly Hills or wound care in Pasadena.
Is Wound Vac Right for You?
If you have a wound that is not healing despite treatment, wound vac therapy may help. This advanced treatment has helped countless patients finally heal wounds that had resisted other approaches.
Talk to your physician about whether negative pressure wound therapy is appropriate for your wound. If you already have a wound vac prescription, our professional wound care team can provide the skilled nursing support you need at home.
Healing is possible. Sometimes it just requires the right tools and the right support to get there.