The most common signs of wound infection include increasing redness that spreads outward from the wound, warmth around the wound, worsening swelling, increasing pain or tenderness, thick yellow or green drainage with a foul odor, fever above 100.4 degrees, and red streaks extending from the wound. A wound that was improving but suddenly worsens is also concerning. If you notice any of these signs—especially fever or red streaks—seek medical attention immediately as the infection may be spreading.
WOUND CARE
Infected Wound Care at Home
Infected wound getting worse? Get expert treatment at home in Los Angeles County. Fast response, certified nurses, antibiotic coordination. Medicare accepted.
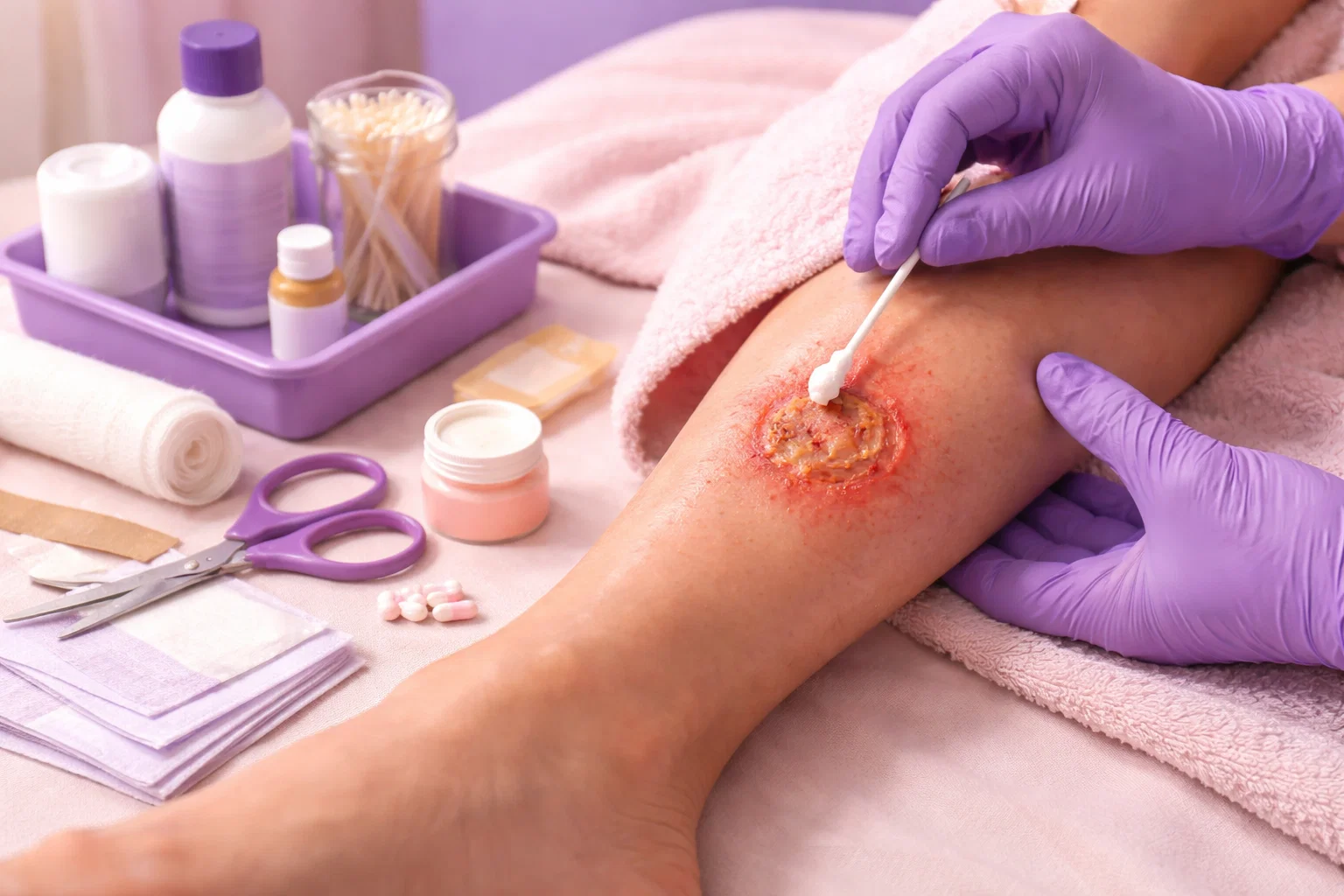
Is Your Wound Infected? Get Expert Treatment at Home Before It Gets Worse
A wound infection is not something to wait out. What starts as redness and swelling can rapidly escalate to cellulitis, abscess formation, bone infection (osteomyelitis), or life-threatening sepsis. Every hour of delay gives bacteria more time to spread deeper into tissue and potentially into your bloodstream.
At HarvardCare at Home, our skilled wound care nurses provide urgent infected wound care throughout Los Angeles County—directly in your home. We identify the type and severity of infection, implement targeted treatment, coordinate antibiotic therapy with your physician, and monitor your response closely to prevent dangerous complications. Medicare, Medi-Cal, and most private insurance accepted.
How to Tell If Your Wound Is Infected: 8 Warning Signs
Not sure if your wound is infected? Watch for these key signs of wound infection:
- Increasing redness — redness that spreads outward from the wound edges, especially in streaks
- Warmth — the skin around the wound feels noticeably hot to the touch
- Swelling — new or worsening swelling around the wound site
- Pain — increasing pain or tenderness, especially if the wound was previously improving
- Purulent drainage — thick, yellow, green, or brown discharge with a foul odor
- Fever — temperature above 100.4°F (38°C) accompanying a wound
- Delayed healing — wound that suddenly stops improving or starts getting worse
- Red streaks — lines extending from the wound toward the heart indicate lymphatic spread
If you notice any of these signs—especially fever or red streaks—contact a healthcare provider immediately. These can indicate the infection is spreading beyond the wound into surrounding tissue or your bloodstream.
Types of Wound Infections We Treat
Our wound care specialists manage the full range of infected wounds at home.
Surgical Site Infections (SSI)
Infections developing after surgery are among the most common healthcare-associated complications. Surgical site infections can involve:
- Superficial incisional SSI — affecting skin and tissue just below the skin
- Deep incisional SSI — involving muscle and tissue around the surgical site
- Organ/space SSI — affecting deeper structures related to the surgery
Early detection and treatment of surgical site infections protects your surgical outcome and prevents reoperation.
Infected Chronic Wounds
Chronic wounds are highly vulnerable to infection due to their prolonged exposure and compromised tissue. We treat infections in:
- Diabetic foot ulcers — where infection can lead to amputation if untreated
- Venous leg ulcers — where bacterial biofilm often stalls healing
- Pressure ulcers — where deep infection can reach bone
- Arterial ulcers — where limited blood flow complicates treatment
Infected Traumatic Wounds
Lacerations, puncture wounds, burns, and other injuries can become infected, particularly when initial wound care was delayed or inadequate.
Cellulitis and Spreading Skin Infections
When bacteria invade beyond the wound into surrounding tissue, cellulitis develops—causing expanding redness, warmth, pain, and swelling. Without treatment, cellulitis can progress to abscess formation or systemic infection.
Wound Infections with Antibiotic-Resistant Bacteria
Infections involving MRSA (methicillin-resistant Staphylococcus aureus) and other resistant organisms require specialized wound management and targeted antibiotic therapy. Our nurses are experienced in managing these complex infections.
What Causes Wound Infections?
Understanding infection risk factors helps with both treatment and prevention:
- Bacterial contamination — all open wounds are exposed to bacteria, but certain bacteria are more likely to cause infection
- Weakened immune system — diabetes, cancer treatment, HIV, autoimmune conditions, and immunosuppressant medications reduce your body’s ability to fight infection
- Poor circulation — inadequate blood flow limits delivery of immune cells and antibiotics to the wound
- Foreign material — debris, dead tissue, or surgical hardware can harbor bacteria
- Biofilm formation — bacteria organize into protective colonies (biofilm) that resist your immune system and antibiotics
- Malnutrition — protein and micronutrient deficiencies impair immune function
- Inadequate wound care — improper dressing technique, infrequent changes, or non-sterile handling
Our Infected Wound Treatment Protocol
We use a systematic, aggressive approach to eliminate infection and restore healing.
Step 1: Rapid Assessment and Classification
At your first visit, we perform a thorough evaluation to determine infection severity:
- Wound assessment — size, depth, tissue type, drainage characteristics, odor
- Infection mapping — documenting the extent of redness, warmth, and swelling
- Systemic screening — checking for fever, elevated heart rate, and signs of spreading infection
- Wound culture — collecting samples to identify the specific bacteria causing infection and their antibiotic sensitivities
- Risk assessment — evaluating factors that may complicate treatment (diabetes, immunosuppression, vascular disease)
This assessment determines whether your infection can be managed at home or requires hospital-level care—and guides every treatment decision that follows.
Step 2: Aggressive Wound Bed Preparation
Infected wounds need thorough cleaning and preparation:
- Debridement — removing dead tissue, slough, and biofilm that harbor bacteria and shield them from treatment
- Thorough irrigation — cleansing the wound bed to reduce bacterial load
- Drainage management — ensuring infected fluid can exit the wound rather than tracking deeper
- Foreign body assessment — identifying any material that may be sustaining the infection
Debridement is especially critical. Biofilm—the invisible bacterial shield present in over 60% of chronic wounds—reforms within 24 hours of disruption, which is why aggressive, repeated debridement combined with antimicrobial therapy is essential.
Step 3: Antimicrobial Wound Therapy
We deploy targeted antimicrobial strategies based on your wound’s needs:
- Silver-based dressings — broad-spectrum antimicrobial activity effective against MRSA, VRE, and biofilm
- Medical-grade honey dressings (Medihoney) — natural antimicrobial with anti-biofilm properties and healing support
- Cadexomer iodine dressings — sustained-release antimicrobial that absorbs drainage and debris
- PHMB (polyhexamethylene biguanide) — antimicrobial cleansers and dressings for wound bed decontamination
- Negative pressure wound therapy — removes infectious fluid and promotes blood flow in appropriate wounds
We select therapies based on culture results, wound characteristics, and treatment response—and adjust as your infection resolves.
Step 4: Antibiotic Coordination
While topical antimicrobials treat the wound directly, many infections also require systemic antibiotic therapy. We coordinate closely with your physician to:
- Communicate culture and sensitivity results for targeted antibiotic selection
- Monitor treatment response and report progress
- Recommend antibiotic changes when initial therapy is ineffective
- Manage IV antibiotics at home when oral therapy is insufficient
- Track for antibiotic side effects and complications
This nurse-physician coordination ensures your infection receives both local and systemic treatment working together.
Step 5: Intensive Monitoring
Infected wounds require close surveillance. At every visit, we:
- Measure and photograph the wound to track progress objectively
- Map infection boundaries to confirm the infection is shrinking, not spreading
- Assess for systemic signs that might indicate worsening
- Evaluate treatment response and adjust the plan accordingly
- Communicate updates to your physician
If infection shows signs of spreading or systemic involvement, we escalate care immediately—coordinating emergency evaluation when necessary.
Why Infected Wounds Are Dangerous
Wound infections can escalate quickly. Here is what can happen when infection is not treated promptly:
- Cellulitis — spreading bacterial invasion of surrounding skin and soft tissue
- Abscess — pocket of pus requiring drainage, sometimes surgically
- Osteomyelitis — bone infection, common in diabetic foot ulcers and deep pressure ulcers
- Bacteremia — bacteria entering the bloodstream
- Sepsis — life-threatening systemic response to infection requiring emergency hospitalization
- Amputation — in severe diabetic foot infections that destroy tissue beyond repair
- Death — sepsis has a mortality rate of 15-30%, higher in elderly and immunocompromised patients
This is why early, aggressive treatment of wound infections is not optional—it is urgent.
Preventing Wound Infections
Prevention is always better than treatment. We educate patients and caregivers on:
- Proper hand hygiene — the single most important infection prevention measure
- Sterile dressing technique — minimizing bacterial introduction during wound care
- Recognizing early warning signs — catching infection in its earliest, most treatable stage
- Blood sugar control — for diabetic patients, tight glucose management dramatically reduces infection risk
- Nutrition — adequate protein and nutrients support immune function
- Keeping wounds covered — appropriate dressings protect against environmental contamination
Why Home Treatment Works for Wound Infections
Treating infected wounds at home provides real clinical advantages:
- Fewer resistant bacteria — hospitals and clinics harbor MRSA and other dangerous organisms; your home is safer
- Faster response time — no waiting for clinic appointments when infection changes demand action
- Better compliance — every treatment happens on schedule without transportation barriers
- Family caregiver training — we teach your family to recognize danger signs and maintain clean technique
- Real-time escalation — our nurses can coordinate emergency care immediately if infection worsens
Insurance Coverage for Infected Wound Care
Skilled nursing care for infected wounds is covered by Medicare Part A for homebound patients with a physician’s order. Coverage includes:
- Wound assessment, culture collection, and skilled nursing visits
- Dressing changes with antimicrobial wound products
- Debridement and wound bed preparation
- IV antibiotic administration at home when prescribed
- Patient and caregiver infection prevention education
Medi-Cal and most private insurance provide similar coverage. Our team handles all authorization and paperwork.
Do Not Wait – Call HarvardCare at Home Today
A wound infection will not resolve on its own. Without professional treatment, it will get worse. Every day you wait increases the risk of complications that could put you in the hospital – or worse.
HarvardCare at Home provides expert infected wound care throughout Los Angeles County. Our certified wound care nurses respond quickly, treat aggressively, and monitor closely until your infection is eliminated and your wound is healing.
Call now for a free consultation. Describe your wound, and we will help you determine the next step. If you need care, we can often begin within 24-48 hours of physician referral.
FAQs
Do you have questions?
Got questions about Infected Wound Care at Home? Here are answers to what patients and families ask most.
Many wound infections can be treated effectively at home with skilled nursing care, appropriate wound management, and oral or IV antibiotics. Infections that require hospitalization typically involve severe systemic symptoms like high fever, rapid heart rate, or confusion, infection spreading rapidly despite treatment, or infections in critically ill or severely immunocompromised patients. Our nurses assess infection severity at every visit and escalate to emergency care immediately if hospital-level treatment becomes necessary.
Untreated wound infections can escalate into serious, life-threatening conditions. Bacteria can spread into surrounding tissue causing cellulitis, form abscesses requiring surgical drainage, invade bone causing osteomyelitis, or enter the bloodstream causing bacteremia and sepsis. In diabetic foot infections, untreated infection is a leading cause of amputation. Sepsis—the most dangerous complication—has a mortality rate of 15-30 percent. Early aggressive treatment prevents these outcomes.
We understand that infected wounds are urgent. Once we receive a physician referral and verify insurance, we can often begin treatment within 24-48 hours. For patients already receiving our home health services, we can intensify care immediately when infection develops. If your wound shows signs of severe or rapidly spreading infection, we will advise you on whether emergency evaluation is needed before home treatment begins.
Antibiotic selection depends on the bacteria causing your infection, identified through wound culture and sensitivity testing. Common options include oral antibiotics like cephalexin, clindamycin, or trimethoprim-sulfamethoxazole for mild to moderate infections, and IV antibiotics like vancomycin or piperacillin-tazobactam for severe infections or resistant organisms like MRSA. Our nurses collect cultures, coordinate results with your physician, and can administer IV antibiotics at home when prescribed.
Biofilm is an organized community of bacteria that forms a protective shield on the wound surface. Over 60 percent of chronic wounds contain biofilm. Bacteria within biofilm are up to 1000 times more resistant to antibiotics than free-floating bacteria, which is why many wound infections persist despite antibiotic treatment. Biofilm requires physical disruption through debridement combined with antimicrobial dressings to eliminate. This is a key reason professional wound care outperforms self-care for infected wounds.
Infected wounds typically require more frequent visits than non-infected wounds. Initially, visits may be daily or every other day for severe infections requiring close monitoring, frequent dressing changes, or IV antibiotic administration. As infection improves, visit frequency typically decreases to two to three times weekly, then further reduces as the wound transitions to normal healing. We adjust frequency based on infection severity and your response to treatment.
Your nurse will provide specific instructions for care between visits. Generally, this includes keeping the wound covered with prescribed dressings, taking all antibiotics exactly as prescribed and completing the full course, monitoring for signs of worsening such as spreading redness or increasing pain, checking your temperature twice daily, keeping the area clean and dry, and contacting us immediately if you notice changes. Never attempt to debride or deeply clean an infected wound yourself.
The most effective infection prevention measures include thorough hand washing before and after touching any wound, using sterile technique during dressing changes, keeping wounds properly covered and protected, controlling blood sugar if you have diabetes, maintaining good nutrition to support immune function, following all wound care instructions from your healthcare team, and seeking prompt professional care for any wound that is not healing normally. Prevention is far easier and safer than treating an established infection.
MRSA (methicillin-resistant Staphylococcus aureus) is a type of bacteria resistant to many common antibiotics. MRSA wound infections are increasingly common and require targeted treatment. Many MRSA infections can be managed at home with proper wound care, appropriate antimicrobial dressings, and antibiotics chosen specifically based on culture sensitivity results. Our nurses are experienced in managing MRSA wounds and use strict infection control precautions to prevent spread to family members.
TESTIMONIALS
What Our Patients & Families Say
AREAS WE SERVE
Infected Wound Care at Home Near You
Our licensed healthcare professionals provide expert care in the comfort of your home. We proudly serve patients and families throughout Los Angeles County.
- A
- Agoura Hills
- Alhambra
- Altadena
- Arcadia
- B
- Bel Air
- Bellflower
- Beverly Hills
- Boyle Heights
- Brentwood
- Burbank
- C
- Calabasas
- Carson
- Century City
- Cerritos
- Claremont
- Compton
- Covina
- Culver City
- D
- Diamond Bar
- Downey
- E
- Eagle Rock
- East Los Angeles
- Echo Park
- Encino
- G
- Gardena
- Glendale
- Glendora
- Granada Hills
- H
- Hacienda Heights
- Hancock Park
- Harbor City
- Hawthorne
- Highland Park
- Hollywood
- Hollywood Hills
- I
- Inglewood
- K
- Koreatown
- L
- La Crescenta-Montrose
- La Mirada
- Lakewood
- Lincoln Heights
- Long Beach
- Los Angeles
- Los Feliz
- M
- Malibu
- Manhattan Beach
- Mar Vista
- Marina del Rey
- Mid-City
- Mid-Wilshire
- Miracle Mile
- Monrovia
- Montebello
- Monterey Park
- N
- North Hollywood
- Northridge
- Norwalk
- P
- Pacific Palisades
- Palms
- Palos Verdes Estates
- Palos Verdes Peninsula
- Panorama City
- Pasadena
- Pico Rivera
- Playa Vista
- Pomona
- Porter Ranch
- R
- Rancho Palos Verdes
- Redondo Beach
- Reseda
- Rolling Hills Estates
- Rowland Heights
- S
- San Dimas
- San Gabriel
- San Marino
- San Pedro
- Santa Clarita
- Santa Monica
- Sawtelle
- Sherman Oaks
- Silver Lake
- South Gate
- South Pasadena
- Studio City
- T
- Tarzana
- Torrance
- V
- Van Nuys
- Venice
- W
- West Covina
- West Hollywood
- West Los Angeles
- Westchester
- Westlake Village
- Westwood
- Whittier
- Wilmington
- Woodland Hills
More Services
In-Home Wound Care Services
- Board-certified wound care nurses
- Personalized treatment plans
- All wound types treated
Diabetic Wound Care at Home
- Diabetes wound specialists
- Blood sugar optimization support
- Advanced offloading techniques
Skilled Nursing Care at Home
- Registered nurses available 7 days a week
- Comprehensive care coordination
- IV therapy and infusion services
 HarvardCare at Home
HarvardCare at Home