Healing time varies based on wound size, location, depth, and your overall health. Small superficial wounds may heal in 4-6 weeks with proper care, while deeper ulcers can take 3-6 months or longer. Factors like blood sugar control, circulation, nutrition, and adherence to offloading recommendations significantly impact healing time. Our nurses track your progress closely and adjust treatment to optimize healing speed.
WOUND CARE
Diabetic Wound Care at Home
Specialized diabetic wound care delivered at home throughout Los Angeles County. Our nurses treat diabetic foot ulcers, neuropathic wounds, and diabetes-related skin complications with advanced techniques. Medicare covered.
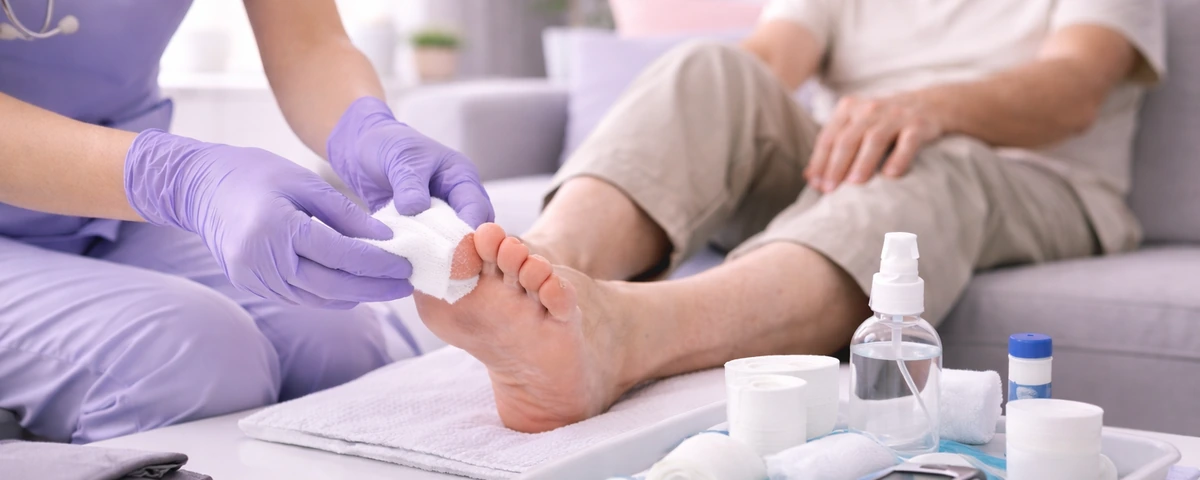
Specialized Diabetic Wound Treatment in Your Home
Living with diabetes brings unique health challenges, and one of the most serious complications diabetic patients face is the development of wounds that heal slowly or fail to heal altogether. Diabetic wounds, particularly foot ulcers, require specialized care from healthcare professionals who understand the complex relationship between diabetes and wound healing. At HarvardCare at Home, our nurses bring this specialized expertise directly to patients throughout Los Angeles County, providing hospital-level diabetic wound care in the comfort and safety of home.
Diabetes affects more than 30 million Americans, and approximately 15% of diabetic patients will develop a foot ulcer during their lifetime. Without proper treatment, these wounds can lead to serious infections, hospitalization, and in severe cases, amputation. The good news is that with prompt, expert care, most diabetic wounds can heal successfully. Our home-based diabetic wound care program is designed to give you access to that expert care without the burden of clinic visits.
Why Diabetes Affects Wound Healing
Understanding why diabetic wounds are so challenging helps explain why specialized care is essential. Diabetes impacts wound healing through several interconnected mechanisms that must all be addressed for successful treatment.
Peripheral Neuropathy
High blood sugar levels over time damage the nerves, particularly in the feet and legs. This condition, called peripheral neuropathy, reduces sensation and makes it difficult to feel pain, pressure, or temperature changes. A diabetic patient might develop a blister, cut, or pressure sore and not even realize it because they simply cannot feel it. By the time the wound is discovered, it may have already progressed significantly.
Neuropathy also affects the nerves that control sweating and oil production in the skin. This leads to dry, cracked skin that is more vulnerable to breakdown and infection. Our wound care nurses assess neuropathy levels and help patients implement protective strategies to prevent new wounds from forming.
Poor Circulation
Diabetes accelerates atherosclerosis, the buildup of plaque in blood vessels. This narrowing of the arteries reduces blood flow to the extremities, depriving tissues of the oxygen and nutrients they need to heal. Poor circulation also impairs the body’s ability to fight infection and deliver immune cells to the wound site.
Our nurses evaluate circulation through physical assessment and coordinate with vascular specialists when needed. Improving blood flow is often a critical component of helping diabetic wounds heal.
Impaired Immune Response
Elevated blood sugar interferes with the function of white blood cells, the body’s primary defense against infection. This weakened immune response means diabetic wounds are more susceptible to infection and that infections, once established, can spread rapidly and become life-threatening.
Delayed Cellular Repair
The biological processes that repair damaged tissue work less efficiently in diabetic patients. Collagen production is reduced, new blood vessel formation is impaired, and the overall healing cascade is slowed. What might heal in days or weeks for a non-diabetic patient can take months for someone with diabetes.
Types of Diabetic Wounds We Treat
Our specialized diabetic wound care program addresses all types of wounds that commonly affect diabetic patients.
Diabetic Foot Ulcers
Foot ulcers are the most common and concerning wounds in diabetic patients. They typically develop on the bottom of the foot, often under areas of high pressure or where shoes rub. These wounds can extend deep into the tissue, reaching muscle and even bone if not properly treated. Our nurses use advanced assessment techniques to evaluate wound depth, check for signs of bone involvement, and develop comprehensive treatment plans.
Neuropathic Ulcers
These wounds occur specifically due to nerve damage and are often found on weight-bearing areas of the foot. Because patients cannot feel these wounds developing, regular foot inspections and preventive care are essential. Our care includes teaching patients and families how to perform daily foot checks to catch problems early.
Ischemic Wounds
When poor circulation is the primary factor, wounds tend to develop on the toes, heels, and other areas farthest from the heart. These wounds often have distinct characteristics and require treatment approaches that address the underlying vascular insufficiency.
Infected Diabetic Wounds
Any diabetic wound can become infected, but the consequences are particularly serious for diabetic patients. Our nurses are trained to recognize early signs of infection and coordinate with physicians for prompt antibiotic treatment when needed. For some infections, we can administer IV antibiotics in the home, avoiding hospitalization.
Post-Surgical Wounds
Diabetic patients who undergo surgery, particularly foot or leg surgery, need careful post-operative wound monitoring. Surgical incisions heal more slowly in diabetic patients and are at higher risk for complications. Our post-surgical wound care helps ensure optimal healing outcomes.
Our Diabetic Wound Care Approach
Successful diabetic wound healing requires a comprehensive approach that goes beyond simple wound dressing changes.
Thorough Initial Evaluation
Your first visit includes a detailed assessment that goes beyond just looking at the wound. We evaluate your diabetes management, including blood sugar control and medication regimen. We assess circulation in your legs and feet, test for neuropathy, examine your footwear, and review your nutrition. This comprehensive picture allows us to identify all factors affecting your healing.
Blood Sugar Optimization
Wound healing is directly tied to blood sugar control. When blood sugar is consistently high, wounds simply cannot heal properly. Our nurses monitor your glucose levels, provide diabetes education, and coordinate with your doctor or endocrinologist to optimize your diabetes management. Even modest improvements in blood sugar control can significantly accelerate wound healing.
Advanced Wound Care Techniques
We utilize the latest evidence-based techniques for diabetic wound management:
- Sharp debridement to remove dead and infected tissue
- Advanced moisture-management dressings selected for your specific wound
- Offloading devices and techniques to reduce pressure on foot wounds
- Negative pressure wound therapy for appropriate wounds
- Growth factor applications and bioengineered skin substitutes when indicated
- Infection management including wound cultures and antibiotic coordination
Pressure Offloading
For diabetic foot ulcers, reducing pressure on the wound is absolutely essential. A wound cannot heal if it continues to bear your body weight with every step. Our nurses assess your current footwear, recommend appropriate offloading devices such as surgical shoes, walking boots, or custom orthotics, and ensure you understand why reducing pressure is non-negotiable for healing.
Infection Prevention and Management
Given the serious consequences of infection in diabetic wounds, we maintain constant vigilance. Every visit includes assessment for signs of infection, and we act quickly at the first indication of problems. Our close relationship with infectious disease specialists and your physician ensures rapid response when antibiotic treatment is needed.
Nutrition Counseling
Your body needs adequate protein, vitamins, and minerals to build new tissue and heal wounds. Many diabetic patients have nutritional deficiencies that impair healing. Our nurses assess your dietary intake and provide guidance on optimizing nutrition for wound healing while maintaining blood sugar control.
The Importance of Early Intervention
With diabetic wounds, time is truly of the essence. A small wound that might seem insignificant can progress rapidly to a limb-threatening emergency if not properly treated. Studies show that diabetic foot ulcers present for more than 30 days before treatment begins have significantly worse outcomes than those treated promptly.
Early intervention also affects cost. Treating a diabetic wound early, before it becomes infected or extends deeper into tissues, is far less expensive than treating an advanced wound or dealing with hospitalization and potential amputation.
If you notice any wound on your feet, legs, or elsewhere on your body, don’t wait to see if it heals on its own. Contact us for an assessment immediately.
Preventing Future Diabetic Wounds
While treating your current wound is our immediate priority, preventing future wounds is equally important. Our care includes comprehensive education on diabetic wound prevention strategies.
Daily Foot Inspections
Because neuropathy may prevent you from feeling wounds develop, visual inspection is essential. We teach patients and caregivers how to perform thorough daily foot checks, what to look for, and when to call for help.
Proper Footwear
Many diabetic foot ulcers are caused or worsened by ill-fitting shoes. We evaluate your footwear and provide recommendations for diabetic-appropriate shoes that protect your feet without creating pressure points.
Skin Care
Keeping skin moisturized and healthy helps prevent cracks and breakdown that can lead to wounds. We provide guidance on proper skin care while avoiding moisture between the toes, which can cause fungal infections.
Blood Sugar Management
Optimal blood sugar control is the single most important factor in preventing diabetic complications including wounds. We reinforce diabetes self-management throughout our care.
Working With Your Healthcare Team
Diabetic wound care requires coordination among multiple healthcare providers. Our nurses communicate regularly with your primary care physician, endocrinologist, vascular specialist, podiatrist, and any other providers involved in your care. We send detailed progress reports after each visit and immediately notify physicians of any concerns.
This collaborative approach ensures everyone is working from the same playbook and that your care plan is continually optimized based on your progress.
Coverage and Insurance
Diabetic wound care services are covered by Medicare, Medi-Cal, and most private insurance plans. Medicare recognizes the importance of home-based diabetic wound care in preventing hospitalizations and amputations, and provides coverage for qualifying patients.
To qualify, you typically need a physician’s order, must be homebound, and require skilled nursing care. Our team verifies your insurance coverage and handles authorization, so you can focus entirely on healing.
Start Your Healing Journey Today
Living with diabetes doesn’t mean accepting poor wound healing outcomes. With specialized care from nurses who understand the unique challenges of diabetic wounds, most patients can achieve successful healing and return to their normal lives.
If you or a loved one is struggling with a diabetic wound anywhere in Los Angeles County, contact HarvardCare at Home today. Our specialized diabetic wound care nurses are ready to bring expert treatment to your doorstep and help you heal.
FAQs
Do you have questions?
Got questions about Diabetic Wound Care at Home? Here are answers to what patients and families ask most.
Absolutely. Most diabetic foot ulcers can be successfully treated at home by specialized wound care nurses. Home treatment often produces better outcomes because you receive consistent care from nurses who know your wound intimately, you avoid exposure to infections at clinics, and you're more comfortable and less stressed. We use the same advanced treatments available at wound centers. Only wounds requiring surgical intervention need clinic-based care.
Infected diabetic wounds require immediate attention as infections can spread rapidly. Signs include increased redness, warmth, swelling, drainage, odor, and fever. If we detect infection, we coordinate immediately with your physician for antibiotic treatment. Many infections can be managed at home with oral or even IV antibiotics. Severe infections may require hospitalization, which is why we emphasize early detection and prompt treatment to prevent infections from becoming serious.
Several factors can prevent diabetic wounds from healing: uncontrolled blood sugar, continued pressure on the wound, poor circulation, infection, inadequate nutrition, or certain medications. Our comprehensive approach identifies and addresses all barriers to healing. Sometimes healing stalls because one factor isn't being adequately managed. We work with your entire healthcare team to optimize every aspect affecting your wound.
Modern wound science clearly shows that wounds heal better in a moist environment, not dried out. The old advice to let wounds air out is outdated. We use specialized dressings that maintain optimal moisture balance, protect the wound from bacteria, and create ideal healing conditions. Your wound should always be covered with an appropriate dressing. Never soak diabetic wounds or apply home remedies without consulting your wound care nurse.
TESTIMONIALS
What Our Patients & Families Say
AREAS WE SERVE
Diabetic Wound Care at Home Near You
Our licensed healthcare professionals provide expert care in the comfort of your home. We proudly serve patients and families throughout Los Angeles County.
- A
- Agoura Hills
- Alhambra
- Altadena
- Arcadia
- B
- Bel Air
- Bellflower
- Beverly Hills
- Boyle Heights
- Brentwood
- Burbank
- C
- Calabasas
- Carson
- Century City
- Cerritos
- Claremont
- Compton
- Covina
- Culver City
- D
- Diamond Bar
- Downey
- E
- Eagle Rock
- East Los Angeles
- Echo Park
- Encino
- G
- Gardena
- Glendale
- Glendora
- Granada Hills
- H
- Hacienda Heights
- Hancock Park
- Harbor City
- Hawthorne
- Highland Park
- Hollywood
- Hollywood Hills
- I
- Inglewood
- K
- Koreatown
- L
- La Crescenta-Montrose
- La Mirada
- Lakewood
- Lincoln Heights
- Long Beach
- Los Angeles
- Los Feliz
- M
- Malibu
- Manhattan Beach
- Mar Vista
- Marina del Rey
- Mid-City
- Mid-Wilshire
- Miracle Mile
- Monrovia
- Montebello
- Monterey Park
- N
- North Hollywood
- Northridge
- Norwalk
- P
- Pacific Palisades
- Palms
- Palos Verdes Estates
- Palos Verdes Peninsula
- Panorama City
- Pasadena
- Pico Rivera
- Playa Vista
- Pomona
- Porter Ranch
- R
- Rancho Palos Verdes
- Redondo Beach
- Reseda
- Rolling Hills Estates
- Rowland Heights
- S
- San Dimas
- San Gabriel
- San Marino
- San Pedro
- Santa Clarita
- Santa Monica
- Sawtelle
- Sherman Oaks
- Silver Lake
- South Gate
- South Pasadena
- Studio City
- T
- Tarzana
- Torrance
- V
- Van Nuys
- Venice
- W
- West Covina
- West Hollywood
- West Los Angeles
- Westchester
- Westlake Village
- Westwood
- Whittier
- Wilmington
- Woodland Hills
More Services
In-Home Wound Care Services
- Board-certified wound care nurses
- Personalized treatment plans
- All wound types treated
Skilled Nursing Care at Home
- Registered nurses available 7 days a week
- Comprehensive care coordination
- IV therapy and infusion services
In-Home Medication Management Services
- Complete medication review and reconciliation
- Drug interaction screening
- Injection administration and training
 HarvardCare at Home
HarvardCare at Home